I had a sleep study done and the report shows OSA that was not well controlled using a CPAP. I reached a low of up to 82% SPO2 with close to 61 AHI. The AHI increased (129) at certain pressure levels on the CPAP. I was prescribed an APAP with the pressure setting between 10 - 20. I have been using the APAP (Resmed airsense 10) for the last 8 days. Here my questions:
Wilson, sounds like the APAP is pretty effective as far as getting the sleep apnea under control. 2.5 AHI ain't bad. Your issue seems to be either the machine function or mask, that is, you are complaining of sleep deprivation. Why are you sleep deprived? The APAP pressure or the mask? Once that is narrowed down, perhaps something intelligent could be suggested. And the next question would be; have you discussed this sleep deprivation issue with the sleep doc?
Hi, I have been using APEX CPAP and the software Easy Compliance 3.0 was used to download the readings from the CPAP. With this software, I can see the detailed compliance graph of the pressure (cmH2O) going up and down during different hours of my sleep, ie. from 4.5 to 7.7 etc. (My daily recordings seldom exceed 8.0 cmH2O, my AHI was 40 dated Feb 2010). Recently, after changing to Resmed Airsense 10 AutoSet, seemed like the only software able to read the downloads is Sleepyhead and this software is not able to show the readings in graph, at which hour pressure was up or down, instead it only show bar graph of the lowest/highest set pressure. Are you able to advise if there are advance/further settings in this software that could be changed? I am also not able to use the ResMed Registered Software as I live in Singapore. Thank you and Best Regards.
You must not be using SleepyHead correctly. It supports the AirSense 10, and I use it. See the chart I posted a little bit further down in this thread. You want to look at the Daily Report. You can zoom in on a particular section by left clicking on it, and then using the arrow keys to zoom in and out, and to move down the time scale. See this guide to SleepyHead:
Wilson, I am just another user of the AirSense 10 AutoSet machine, and not a professional. So don't take this as professional advice. It is simply that of another user.
Yes, your APAP is doing a pretty good job in reducing an AHI of 61 down to a residual AHI of 2.5. An AHI in the 0-5 range is considered normal. That said, an APAP is normally more effective in reducing obstructive apnea than it is in reducing central apnea. What portion of that 2.5 AHI is obstructive and what part is hypopnea? In my experience I think hypopnea can be related to obstructive apnea, or central apnea. So, I always look at the hypopnea component as a bit of a question mark.
An APAP tries to normalize obstructive apnea and obstructive hypopnea by keeping the airway open with air pressure. That physically usually works, but it can have some side effects. Mask discomfort is usually the worst one. I have tried 5 different masks and finally settled on a nasal pillow mask. That said masks are very personal and I really can't give you any advice other than to keep trying ones to the extent you can. What I can say is that about the second worst sleep I ever got was my first night with an APAP. The worst night was when I did the at home sleep study. Both terrible sleeps. But, I have slowly gotten used to wearing a CPAP at night and the benefits are now outweighing the initial discomfort and the effect it had on my sleep quality. In short, give it some time. And if a mask is not working for you, ask your supplier to suggest another. You also mention that you have obstructive apnea that is not well controlled with pressure. That is unusual. You may want to ask your general practitioner to refer you to a specialist to see if there are other reasons for obstruction. In my understanding of risk factors, your age and BMI should not put you at high risk of OSA, so there may very well be another reason.
Some general comments. You said your AHI went up to as high as 129 at certain pressures. I would ask your sleep doctor or sleep tech what the reason for that could be. In some people central apnea goes up when pressure goes up. It would be helpful to know if that applies to you. At the same time you could ask if it is a pressure in the 10-20 range that you have been prescribed, and could be a contributor to your residual AHI if the machine runs you all the way up to 20 cm.
Many people who suffer from apnea track their results on SleepyHead. It can be very informative as to what may be affecting your sleep quality, and how well the machine is working for you. If you are interested I can post some more information on it. In my opinion as a user, the ResMed supplied MyAir applications is not very good. SleepyHead is much better.
Hope that helps some. Any questions, just ask.
Thanks for your responses. When my split study was done, I had one CSA event without the CPAP and two with the CPAP. The doctor did not think that was significant to show CSA. My sleep report shows AHI of 2.4. Total AI of 1.7 and central AI of 0.9 with a pressure of 14.5. I have not discussed my sleep deprivation with the doctor yet. I was waiting to check the nasal mask first. I do believe that the discomfort is coming from both the mask and the pressure. When I start my sleep with pressure set to 6, I feel pretty comfortable but I seem to waking up frequently when pressure is higher and I remove the mask at times.
Interestingly I gargled with warm saline water last night and I slept much better. My events per hour over an usage of 6.5 hrs. dropped to 0.5. I did use a wearable SPO2 monitor before I did the sleep study. The result was consistent with the sleep study. The report from the SPO2 monitor showed couple of lows up to 82% how ever my average SPO2 was at 94%. I am waiting for my nasal mask to arrive to see how that goes. Meanwhile I will continue using the full face mask. Is there a way for me to look at a more detailed report using sleepyhead from data that is on the Resmed APAP or do I need to use a wearable SPO2 monitor?
Thanks!
Yes, you can get a much more detailed report out of SleepyHead. You need a PC or Mac, and a SD card reader. After you install the software you can take the SD card out of the ResMed and transfer the data to SleepyHead. It should help you identify opportunities to see if the pressure can be adjusted. I will post a screen shot below as an example of what you will see. You can download SleepyHead at this link. It is freeware. And here is a link to a basic manual. Depending on your model of SPO2 monitor you may be able to display that data too. Click on the Oximeter link on the main SleepyHead page for more info.
Are you using the EPR feature? If so you may be able to gain a maximum mask pressure reduction by simply turning it off. Both myself and my wife use EPR at 3 but only during the ramp period.
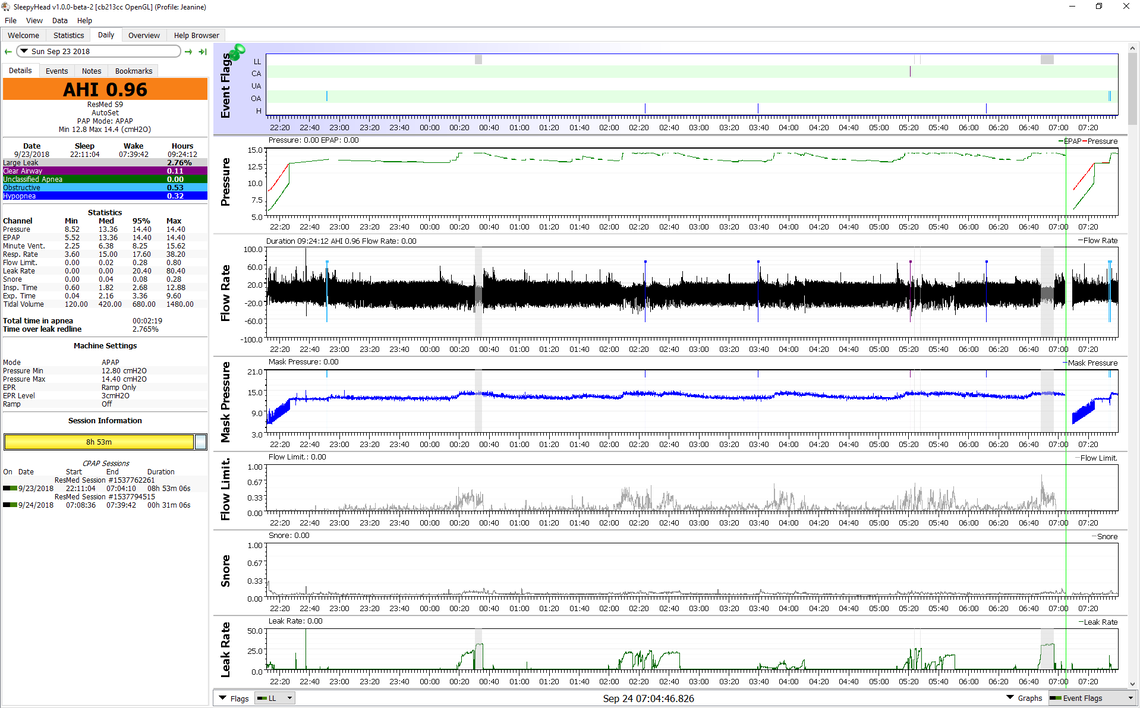
Here is a screen shot from my wife's ResMed S9. She runs a pressure a little higher than mine, and close to what you have. She objects to the higher pressure so it is limited by the maximum pressure setting. Her values are min 12.8 and max of 14.4. This is not quite enough to totally control the flow limitations, but she dislikes having it higher, and over the longer term averages an AHI of about 1. She is currently using a F&P Brevida nasal pillow mask. It generally works well, but she does get some significant leaks during the night for short periods of time. I suspect from what I can hear that she dislodges it out of place to cause the leak.