Hi All
I had been suffering from migraines and TMJ since 2008. Finally in 2018 I was diagnosed with UARS. I tried everything from nasal dilators to MAD devices and then I started doing radio and laser therapy on my soft plate and nose (its very narrow and I weigh 56 KG). Anyways finally in September of 2019 I started CPAP- it was like a miracle my migraines went down from daily to like twice a month. my fast heart rate and irritability went away. My pressure was at 5-12. Also I was on Nexium for severe LPR about 40 twice daily. I take melatonin and Claritin but when I started getting better I stopped the Claritin and went down on the melatonin (was feeling still perfect) then went off the Nexium end of November.. In January my symptoms returned full-fledged. I wondered if it was due to the LPR contributing to the apnea or vice versa so went back on it just right now. suddenly nothin is working. I use the4 dreamer pillow tried switching to a full face mask for few days I felt worse and then I switched to nasal pillows which seem to be fine but my symptoms are not goin away. Please help!
Hi Sierra I just realized this reply has been hidden! for some reason I can't post any photos but in general AHI is between 1.5 and 2 but I began feeling horrible since January. For example yesterday had 4 flow limitations. 12 hyopneas, 4 obstructive and one VS2. they vary from day to day.
Ok, for an 8 hour sleep the 12 hypopneas and 4 OA's would work out to an AHI of about 2. That is a bit high for most, but well under the <5 guideline for treatment. I would worry less about the flow limitations, and not at all about the VS2's. Nobody is really sure what they mean. I gather you have a DreamStation machine?
What you might consider is downloading the OSCAR software to have a more detailed look at when you are having your events, and at what pressures you are having them. It should give you some idea if there is any opportunity for improvement. The software is free, but you need a PC or Mac and a SD card reader to get the data off your SD card in your machine.
Hi Sierra I have been using Oscar and have charts but for some reason I can't upload the images here.
I also noticed you recommended to someone with UARS to do the following (pasting it from another blog). What is this for me? is this c or a flex? and at what number should I put the flex? I have set it off last two days but I suspect its making my tmj worse but it could all be in my head.... I have already increased pressure to 7 as of yesterday...
Ramp Time: Auto - This will hold the initial ramp start pressure until the machine decides you are asleep Start Pressure - I would set this to 7 cm. This will ensure you are getting enough air to not get a suffocating feeling while going to sleep. You normally want the start pressure to be high enough that it feels easy to breath. If this seems like too much then set it lower. The start pressure cannot be higher than your minimum pressure, so to do this you would need to adjust your minimum pressure up to match your start pressure. EPR: On EPR Type: Ramp Only. This will cut the pressure back on exhale only while you are awake. After you go to sleep it will stop the cutback and make the pressure more effective. Since you need so little pressure you could also try it with the EPR on full time. EPR Level: 3 cm. This will drop the pressure 3 cm on exhale until you go to sleep. This makes it easier and more comfortable to get to sleep. If you switch the Type to full time, then it will do this all night.
If you have a DreamStation you will not be able to follow those suggestions exactly. They are for a ResMed machine. The DreamStation does not have the ability (to my knowledge) to use Flex on the ramp only. I believe you have to set it on or off. Turning Flex off may keep your pressure a little lower when in Auto.
What I would suggest is looking at OSCAR's Daily report, and look to see when obstructive events are occurring relative to the pressure. Unfortunately the ability to upload a screen shot to this site seems to have been disabled. However, if you look at the period of time when the pressure is in auto mode after the ram is over, there may be times when the pressure is not very high, but you are still having obstructive events. The DreamStation machine tends to bump the pressure up when it sees an event. Then after the pressure goes up, the pressure goes down fairly shortly later. It waits to see if more events occur. It keeps testing to see if the pressure can be lowered. The net result of this is that a DreamStation machine ramps the pressure up and down very often. This can cause more events to occur than if it just ramped pressure up and held it longer. That is basically what a ResMed does. You can take this up and down pressure out of the machine by boosting the minimum pressure to prevent the machine from doing it.
The other thing to check for is if the pressure goes up to your maximum and you still see obstructive events when at this maximum pressure. This suggests your maximum pressure may be too low, and needs to be increased. This said I would suggest getting the minimum pressure optimized first. Then if that is not enough, then as a second stage adjust the maximum if necessary
HI Sierra you are a life saver thanks for the advice- I appreciate it.... Ok I hope I'm reading it correctly its quite confusing but examples
had a flow limitation at 2:30 and right after pressure went up to 9.7 then down again to 7 after about twenty minutes are so but had an OA at about 2:48 so pressure was still 9 and stayed there and eventually went back down to 7... but sometimes there are no events and it goes up to 8.50 then 9 I continue to see this.. so for example I had an OA at 6:47 in the morning but pressure stayed at the minimum pressure 7. (I have bumped up pressure from 6 to 7 last two nights) However, in terms of maximum pressure I don't think I can see it every going above 10 (maybe just one day it was at 11 in February that's it).right now my maximum is 12. So I guess since I have bumped it up to 7 should I stay like this for a few days (total of a week to try it out or what?) then bump it up more if I still feel horrible? I also noticed woke up from opening my mouth I think I am doing that too. The only difference between minimum pressure 7 and 6 is I slept throughout the night....
The column is getting a bit narrow, so I will post here. From what you describe it sounds like minimum pressure could be increased some more and the maximum reduced to 10 cm. If you are OK with the minimum pressure higher, you may be best to have a minimum of 9 cm and maximum of 10. However you are probably best to increase the minimum in steps of 1 cm to see how you are liking it. Reducing the max to 10 could be done right away. Just watch that you are not hitting that max very often. It really only needs to be increased if you are hitting it and still having some obstructive events when it is at that maximum.
With increasing minimum pressure you should see fewer flow limitations and fewer obstructive events as the up and down cycle in pressure is reduced.
Hi Sierra
Image upload is now working... I have been increasing the minimum by 1 cm every week. Felt no difference at 7 but a huge difference at 8... almost like a 70% difference... but I still wake up a few times... Now I am thinking to bump it up to 9. My question is about the maximum I haven't really touched it... It seems on three of the days it went up to about 12 but not sure why it never went up to 12 when my minimum was lower. I posted an example of when it goes up to 12- you can see my breathing doesn't seem normal but the machine doesn't really record it as anything... if you see the one dated 26th at around 6am- this is a frequent thing that happens where I wake up and then when I check I see weird lines but no recorded event.. I am assuming I still should take it up to 9 but what should I do with the maximum? keep it as is? Thanks so much!! Let me know if you need any other images...
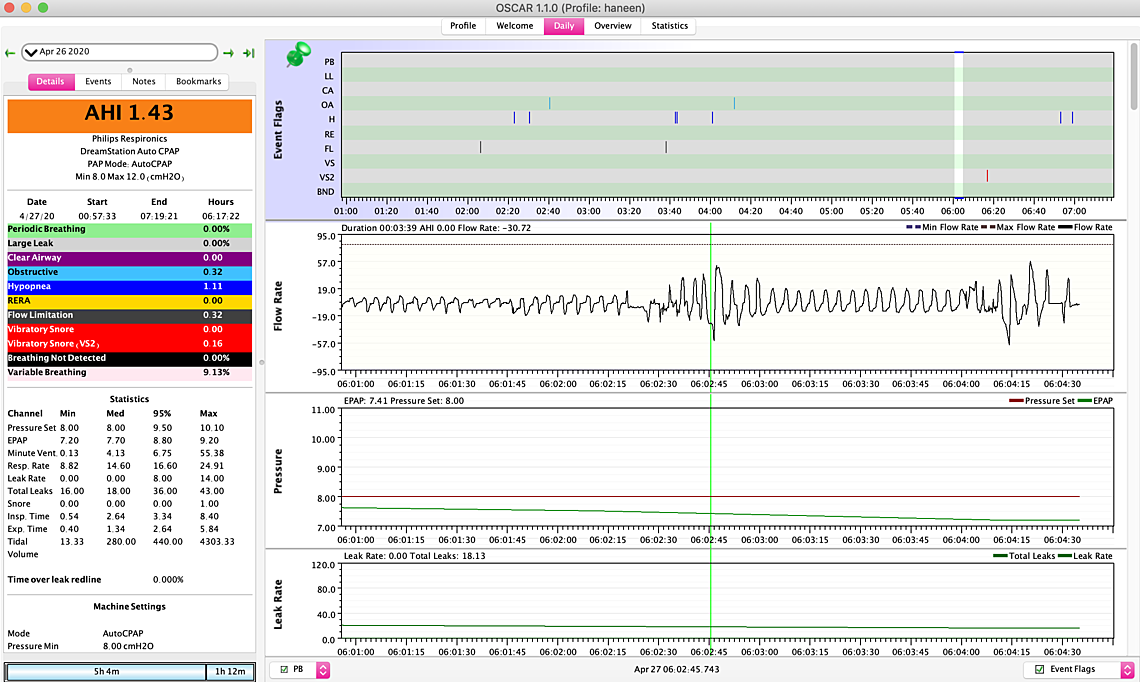
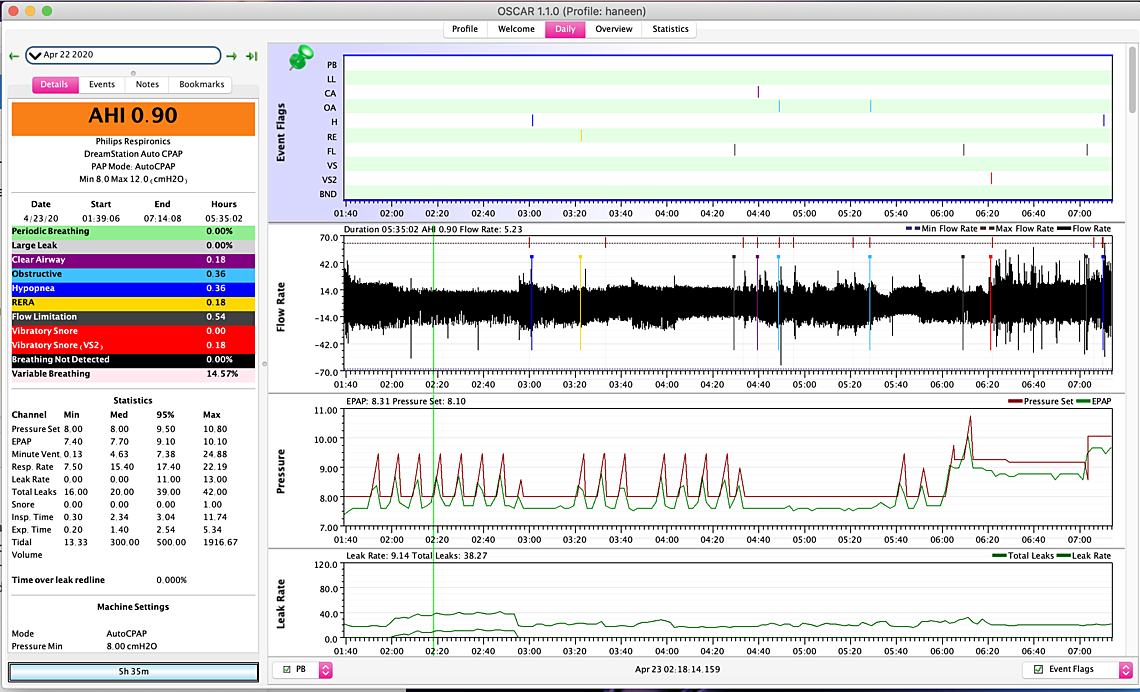
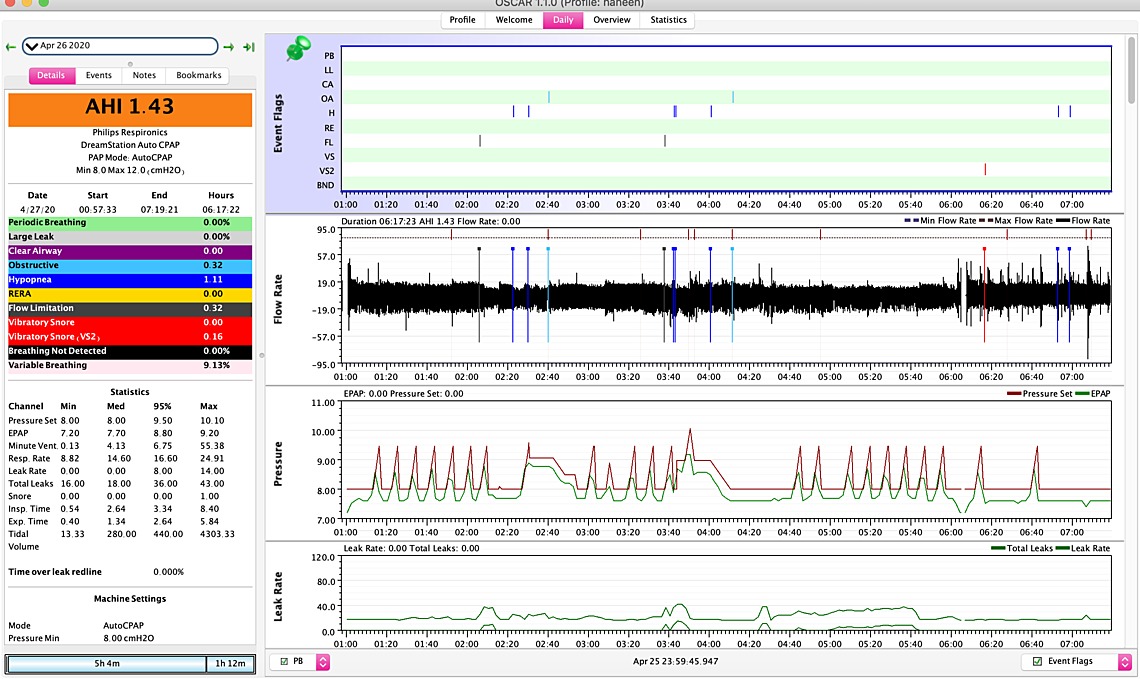
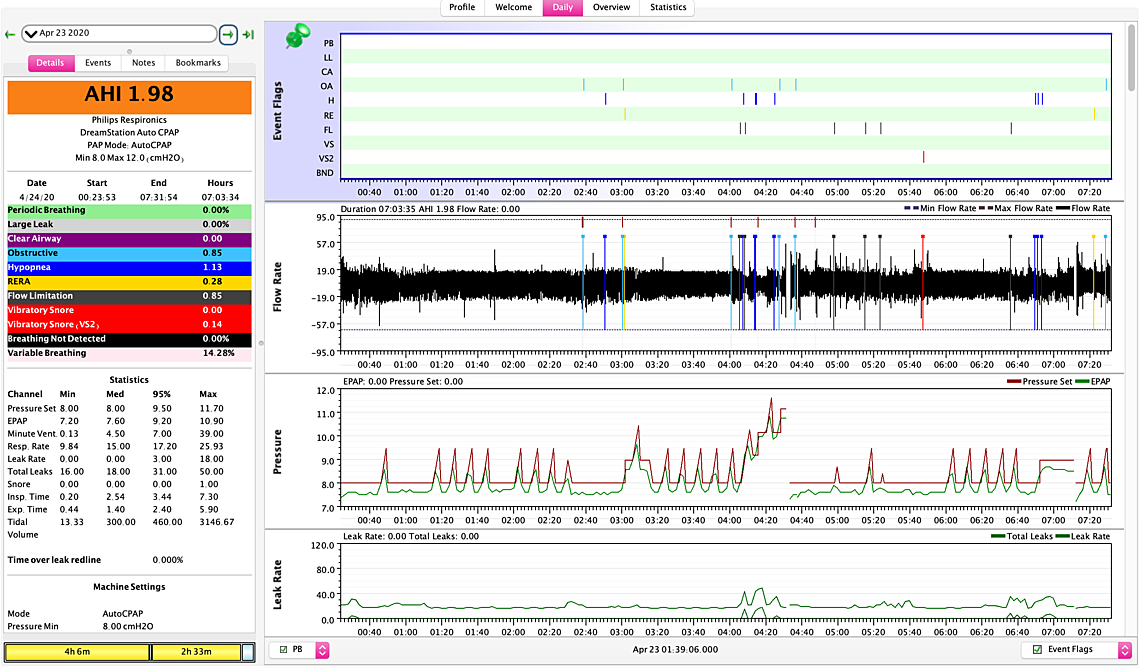
Your graphs are pretty typical DreamStation results. The spikes in the pressure curve are what some call the "hunt and peck" signature of DreamStation. It is kind of like a chicken aimlessly wandering around the yard pecking away to see if there is something good to eat or if it is a stone. I believe the purpose is to raise the pressure to see if your breathing improves. If it doesn't then it drops the pressure back down again. The up side is that it on average keeps your pressure lower. The down side is that it causes the pressure to vary during the night, which may disturb the sleep of some. The other down side is that when the pressure is at the lower value you can have events. See this snip of your April 22 night. I highlighted three events, one hypopnea and two obstructive, that occurred when the pressure was at the 8 cm minimum. These are the kind of events you may potentially avoid if you increase the minimum to say 9 cm. You also appear to be using some Flex (green pressure trace), and you would gain a little bit by turning that off. On exhale it is reducing your pressure below 8 cm.
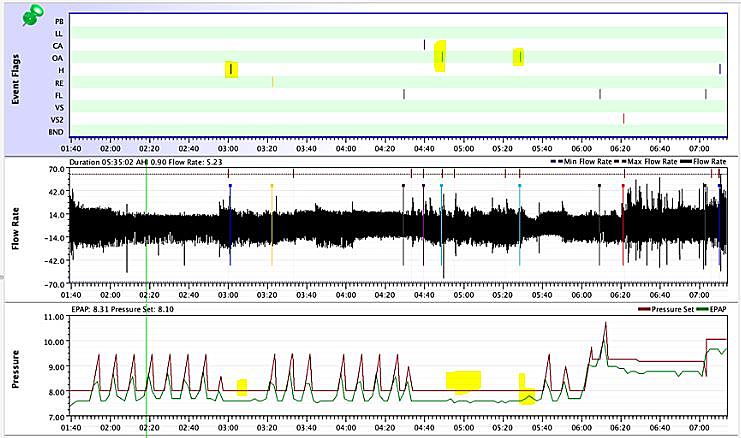
As far as reducing your maximum, it looks to me that it is not doing any harm (or much good) where it is now. One advantage of reducing it to 10 cm with the minimum set at 9 cm is that it would limit some of the hunt and peck spiking of pressure. There may be a comfort gain in that. Also on the 23rd, I see that pressure went up, and it looks like you may have woken up and shut the machine off? Perhaps the extra pressure disturbed you? The machine however was properly responding to both obstructive and hypopnea events. If the machine had been constrained to 10 cm max it is hard to say if that would have made those events worse or not. I would estimate it would not. And if Flex had been turned off, the events may have even been reduced.
The zoomed in trace on the 22nd, looks to me like a normal waking up and falling back to sleep event. I would say nothing to be concerned about.
My thoughts would be to turn Flex off and increase the minimum to 9 cm, then see how that works. A second step if all is good, would be to try reducing the max to 10 cm to see if that helps with controlling the pressure spikes.
Hi Sierra
Thanks for all the information. You have a been a true life saver- I hope I can repay the favor! Usually when I turn it off its because I woke up from something with my heart racing... I usually then go back the next day and see if I had an event that made me wake up like that.
I will try to turn off the flex- but the reason that I had turned it on is because I watched Dr. Barry Krakow's youtube video on using c flex for UARS patients. Any thoughts on this?
https://www.youtube.com/watch?v=rOophPt7DxQ
It won't hurt to turn it off though. I will definitely raise it to 9 today and turn off c flex and then see from there..
again, thank you, thank you, thank you
Without getting into the real detail the DreamStation CFlex and FLex systems really do not reduce pressure that much on exhale. They more smooth the transition between inhale and exhale. The ResMed makes more of a real change in pressure. The setting more closely match the actual pressure drop.
I watched the video. The problem I have is I don't know how you measure UARS. I believe it is thought to be a narrowing of the airway but not a blockage. If that is the case it may cause hypopnea, or flow limitation. A ResMed machine gives you a continuous readout of flow limitation, but I believe the DreamStation only flags FL events. If so, with the DreamStation you could look to see if hypopnea events and FL events are reduced with more Flex or not. The other consideration is that if UARS is actually a narrowing of the airway, reducing the pressure may make it worse, not better. So, I really did not see the point that the author of that video was trying to make.
A BiPAP uses much more of a pressure difference between inhale and exhale. It is more of a breathing assistance device to increase the air flow, than it is an airway splint or opening device. With a BiPAP you can have 10 cm or more of pressure support, compared to the less than 1 cm your graphs are showing for the Flex effect.
About the only way to see is to try it. Hope that helps some.
That does help.. I couldn't sleep with it on so I turned it off after an hour of tossing and turning.. Ill try to turn it off again today...also I have been getting really bad aerophagia I woke up with what felt like really bad burping and my mouth was super super dry. It impossible I should it lower it by a half cm or back to 8? or lower the maximum pressure?
Yes, if you are having issues with the pressure, then it would be good to try going up in lower steps. Perhaps try 8 cm with no Flex first, and when you are used to that, try a small step toward 9 cm. In the scheme of things 8-9 cm is not a very high pressure. When you need 20-25 cm then it can be much more of an issue. Most BiPAP machines go up to 25 cm.
Have you tried a ramp for going to sleep? I am less familiar with the DreamStation machines, but I think they have an auto ramp feature like ResMed. It holds the pressure at a set level until it senses you are asleep. If it does, you may want to try a ramp hold at 7 cm. That may be easier to get to sleep with.
Yes I have a ramp I will set it at 7. ill increase it by 0.5 cm every week and see... and ill try the no flex first... thanks so much
You may want to try the SmartRamp feature. It is described on pages 4-22 and 4-23 in the manual at the link below. If I understand it correctly it will control the pressure automatically between the ramp start pressure selected and the Auto Minimum pressure, until the ramp time expires. Again if I understand it correctly, unless it encounters a OA or H event it will keep the pressure at your ramp start pressure. For a 8 cm min pressure you could try the SmartRamp with the Start pressure set at 7 cm. And when you try the 8.5 or 9 minimum Auto pressure perhaps leave the Ramp Start at 7 cm if you find that comfortable.
This works a bit differently than the ResMed and the manual applies to all models of the DreamStation so that makes it a bit difficult to understand. The ResMed just hold the pressure at the Ramp Start until it detects you are asleep. It appears the DreamStation will kind of hold it, but will stay in effect until the ramp time expires.
thanks so much this information is ten times more helpful than any doctor has ever provided me. I will look into this today. any advice on what to do if im snoring (not too much just a few times per night (last night was twice but one time it woke up) I rinse with netipot nightly so im not sure if I should go back on cortisone sprays or try mouth taping (I only tried most taping for two nights so not sure if it works for me) or try a full face mask? or just leave it alone for now and maybe as I increase the pressure this might help?
On the snoring, my observation is that the pressure needed to stop the obstructive apnea generally is enough to also stop snoring. My wife has some issues with snoring and flow limitations showing up on SleepyHead that are not quite totally controlled by the pressure she uses (ResMed S9). They can be controlled with more pressure, but she does not want to use any more pressure, as it wakes her up. So, I limit the pressure so her AHI scores are very good (averages under 1.0), but it is not quite enough to stop the flow limitation. See the example of her daily report below. Not sure if the DreamStation responds to snoring. Suspect it does to flow limitations though. In short I would not worry about it until you have gotten the pressure up a little higher and your score is better. It will probably go away. Mouth taping generally only stops excessive leakage from air loss through your mouth. It probably wouldn't do much for snoring. Neither would a full face mask. From the reports you have posted I have not seen a high leakage. DreamStation provides two leak rates. The top one included the intentional flow out the mask vent. The bottom one is more representative of the unintentional leak. That is the one to be concerned about.
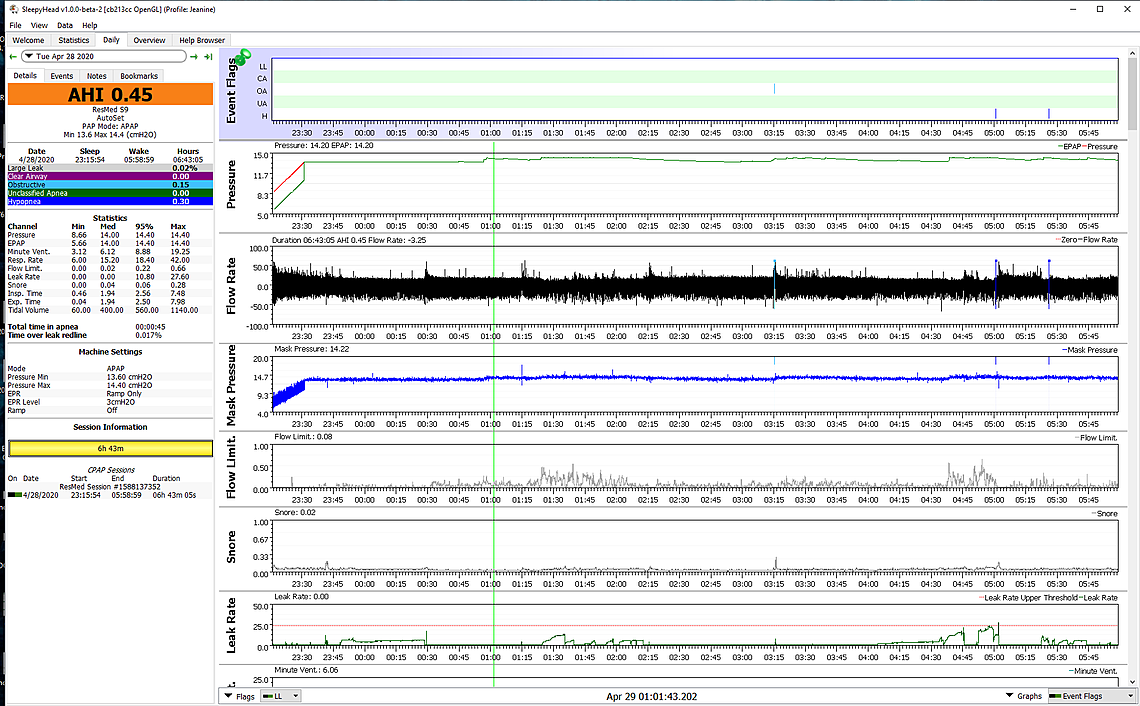
yea I still can't sleep that well even at the 8 but wow I feel so much better in terms of the migraines and tmj and energy. im sleeping less like 6 hours which is weird that I have more energy but still waking up around 5 or 6 and then can't go back to sleep - I am hoping I will adjust I might take some melatonin in the meantime see if that helps.
I'm sure you will get used to the pressure over time. I used to think 6 cm was a high pressure when going to sleep. Then I discovered that it was actually low. When you first go to bed and are breathing more deeply it can kind of restrict the air flow. Over time I adjusted the Ramp Start pressure which is used when going to sleep. I kept increasing it until I could feel no flow restriction when breathing deeply. At the right pressure it feels like there is no mask on your face, and nothing restricting flow. Now I am at 9 cm for my ramp start and find it quite comfortable.
Because I used a fixed pressure after the ramp is over set at 11 cm, that is what is there if I wake up during the night. It would be nice if it would sense I was awake and start the ramp over, but it does not. It only does that if I shut the machine off for a few seconds. I had a Trial F&P machine and it had a "SenseAwake" of something like that, that did sense you were awake and ramped the pressure back down. However that was about the only good feature of that machine. But again over time, I now find a fixed pressure of 11 cm quite comfortable. The only irritation I get from my mask are the straps.
Short story, you will likely adapt to the pressure...
Thanks so much for sharing your experience - when do you recommend I raise it more though? I could do 0.5 increments. every week or two by a 0.5 cm maybe? thanks so much its been about 5-6 days on pressure 8. so for April 30th I woke up at 5:45 no idea why... and for the third woke up at 7:06 for no reason... my biggest problem is waking up at around these times and not being able to sleep it happened even before the pressure thing.. I think I am ok at 8 right now in terms of falling asleep with pressure and ramp at 7.5 - the question is do I bump it up a 0.5 for another week perhaps with a ramp at 7.5 again?
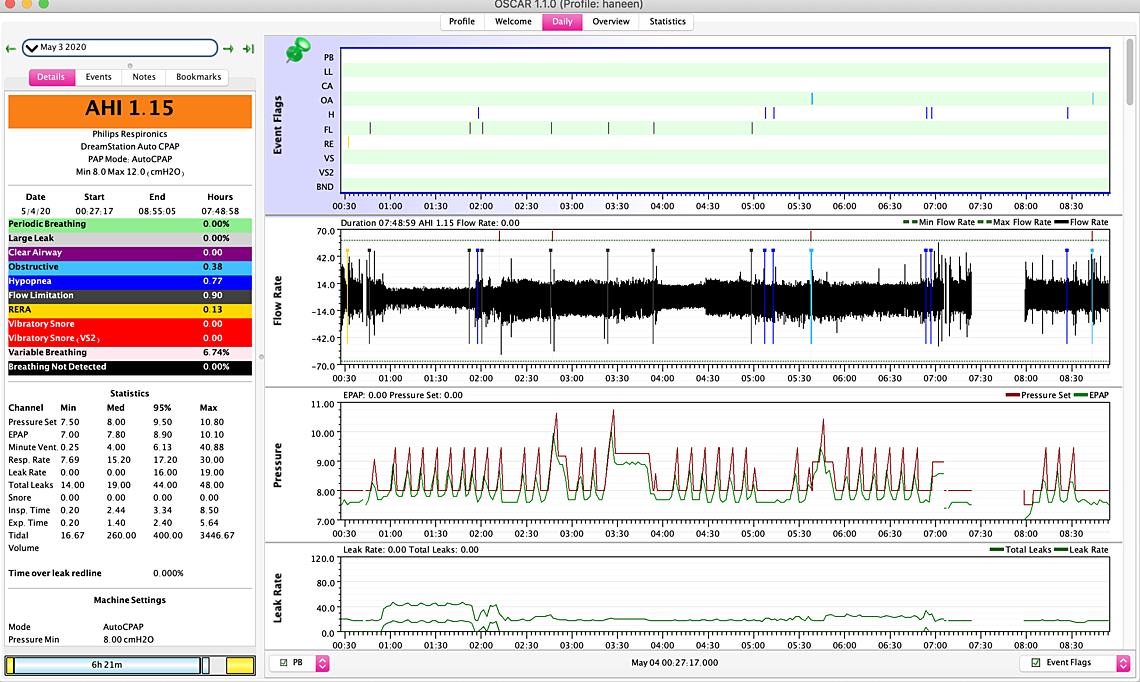
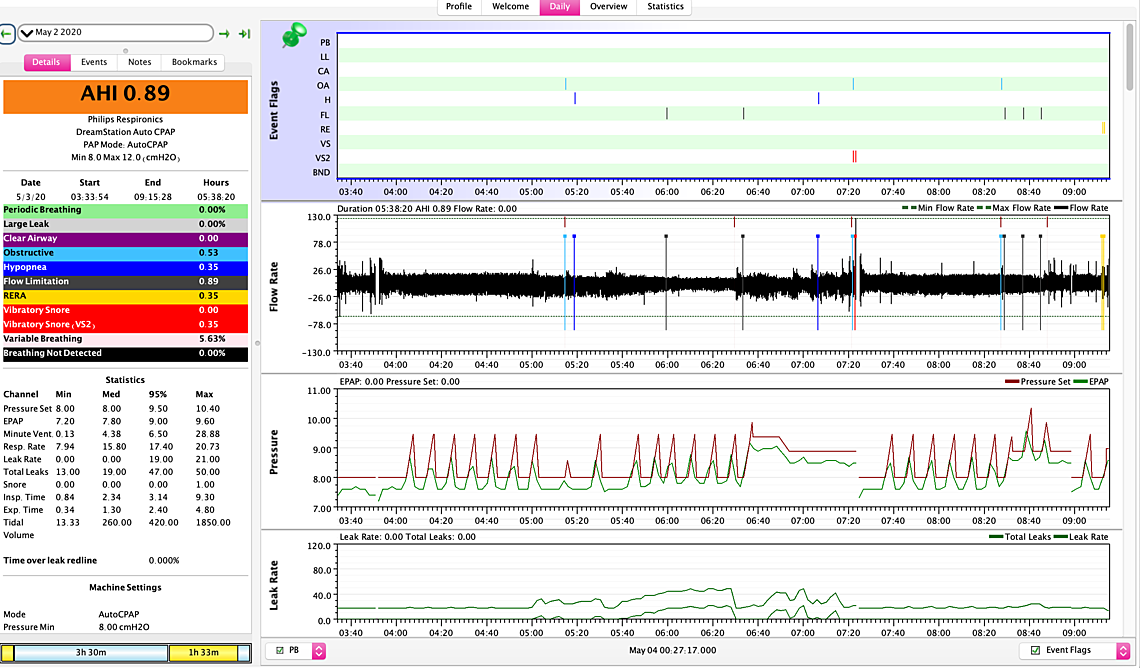
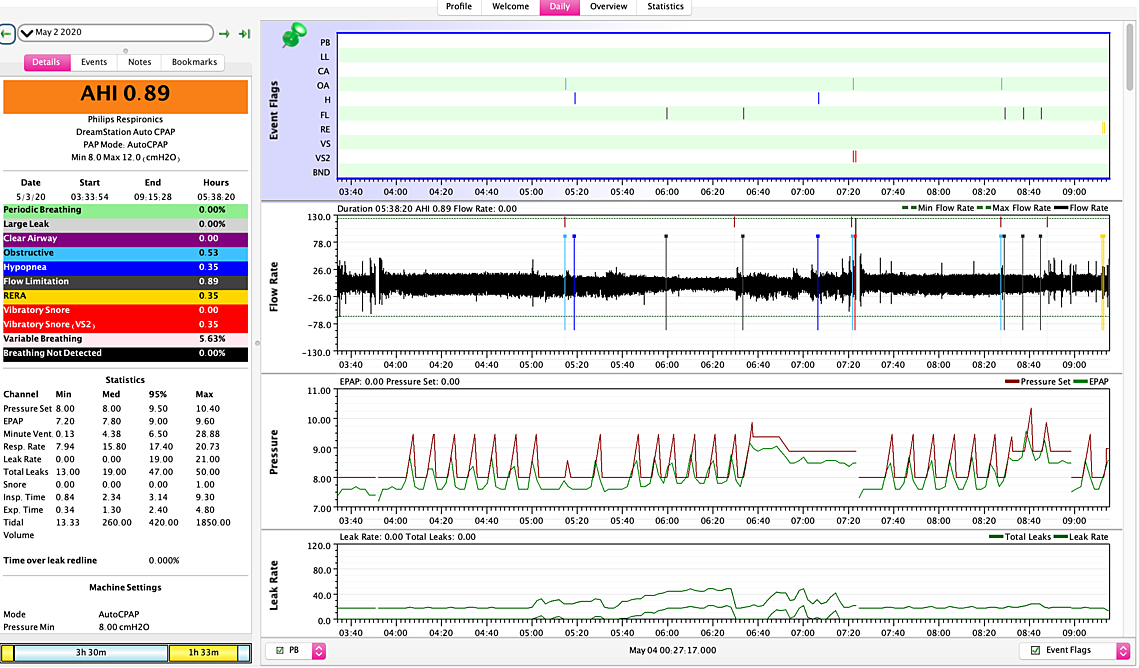
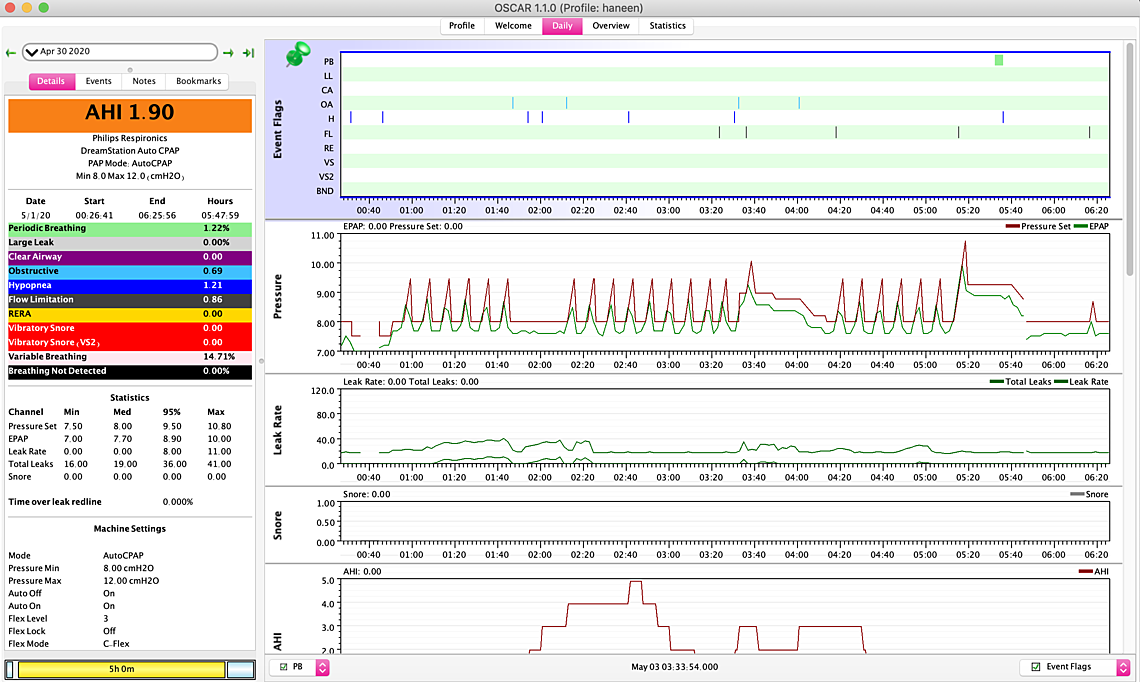
Some thoughts:
will try to turn off flex today and report back soon with results. as for the periodic breathing I just checked it happens like once a month so I am assuming that is ok. I will try to turn the leak feature on I have a Mac so I need to fiddle with it a bit.
Thank you so so much
If you check what the flow curve looks like when expanded for the PB area you will get some idea what it looks like. Then if you check your hypopnea events you may find some of them that look like the PB but are flagged as H events. So the issue may be a bit more significant than it looks at first look. That said, it is difficult to do anything about it with a CPAP. I get the issue about once a month also, and don't worry about it a lot. This is what my last Cheyne-Stokes event looked like. The part I circled in red is pretty classic.
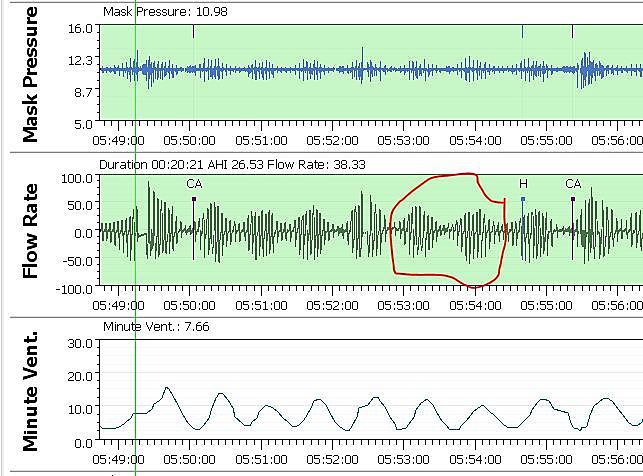
Hi Sierra
So I reduced my Nexium dosage from 40 mg to 20 mg a few days ago but I also turned off the c flex and took a melatonin last night. Now I feel horrible again any idea to which one is causing this? I literally have had a racing heart all day and a migraine tmj that's when I know I had a horrible night - which makes sense cause I have more events on Oscar.... this is the second day I feel horrible so I am suspecting its not the c flex but maybe either the melatonin or the Nexium.... I usually have had a history of bad LPR ...
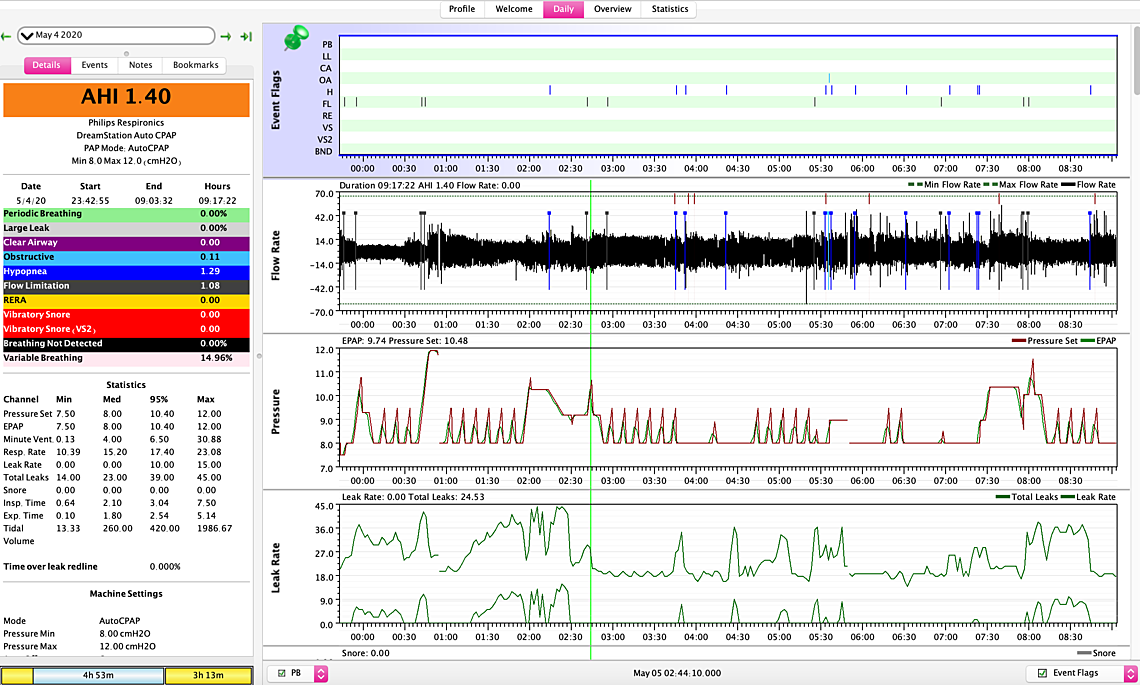
Hello,
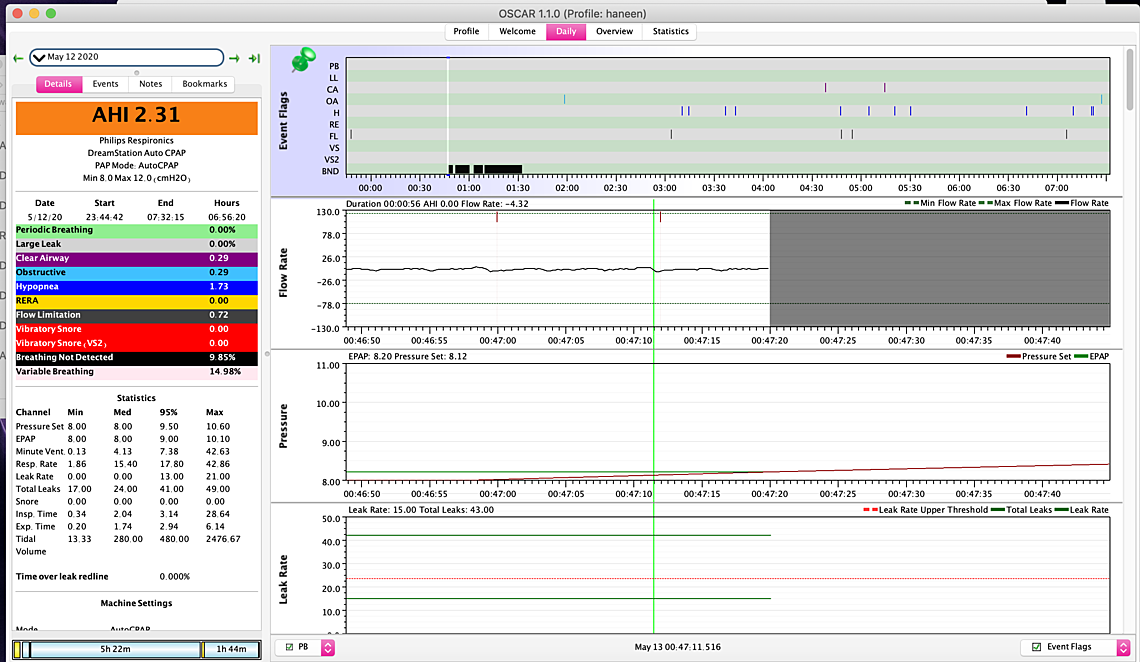
So here are some updates: First I'm not sure if am reading my charts correctly... for example on this May 8th (see attached) I had four or five hyopneas in a row (5 am)but pressure was at 9.6 so I am wondering does this mean I still am not at the ideal pressure…. Also between 12:30-1:30 barely had anything pressure was at 10 I am assuming is this why? I want to know if my readings are correct…. I went back on Nexium on May 8th I highly suspecting my GERD is not helping at all …. the headaches magically disappeared since going back on the 40 mg dosage.. I still have symptoms though but the headaches went down significantly... I also couldn’t handle the c flex off but I might try going down to tonight and see if I can handle it…. Its either do that or try to go up from 8 to 8.5 - I think tonight I will turn off the c flex or increase to 8.5 ... Now the problem I am facing is on the 9th and 10th I didn't use the Cpap because my eyes were so dry I felt like my eyes were gonna crack open and my forehead was all irritated - so I used my MAD device instead... was ok first day but second day a bit of jaw popping... I made sure last night I slept without a pillow in front of me are anything that could direct air back into my face... but my eyes are bad again tonight... I thought bringing pressure down from 8.5 to 8 would help but it didn't.. I am gonna switch to my nasal pillow tonight instead of y nasal cushion and see if that helps but im also suspecting that im opening may mouth (is this possible considering I don't have significant leaks) was thinking of taping my mouth to see if that resolves.... I just have this feeling the cpap isn't recording my mouth leaks.. also on the 12th I have this stopping breathing thing which is quite odd.... - I uploaded a close up of the flow rate im suspecting mouth breathing...
Thanks so much !
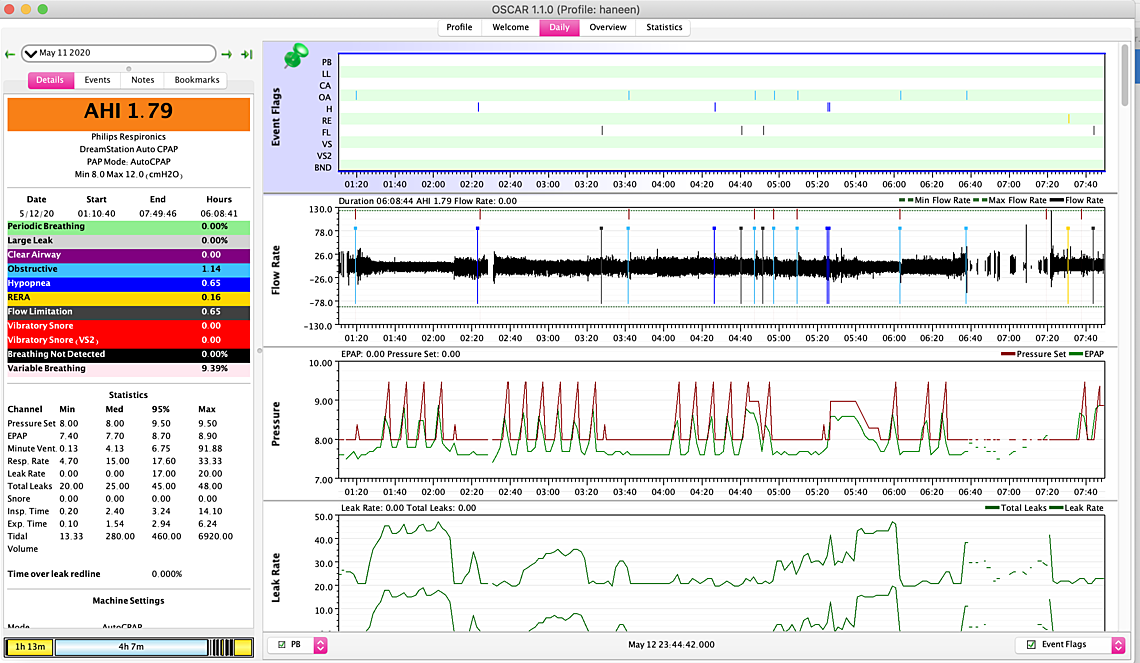
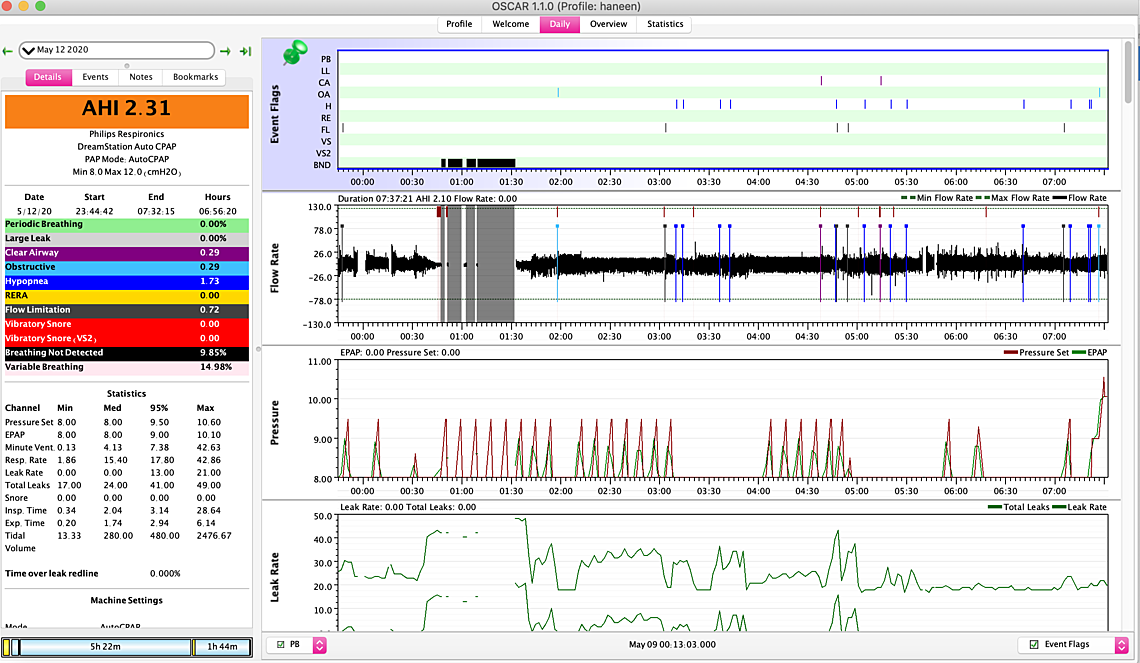
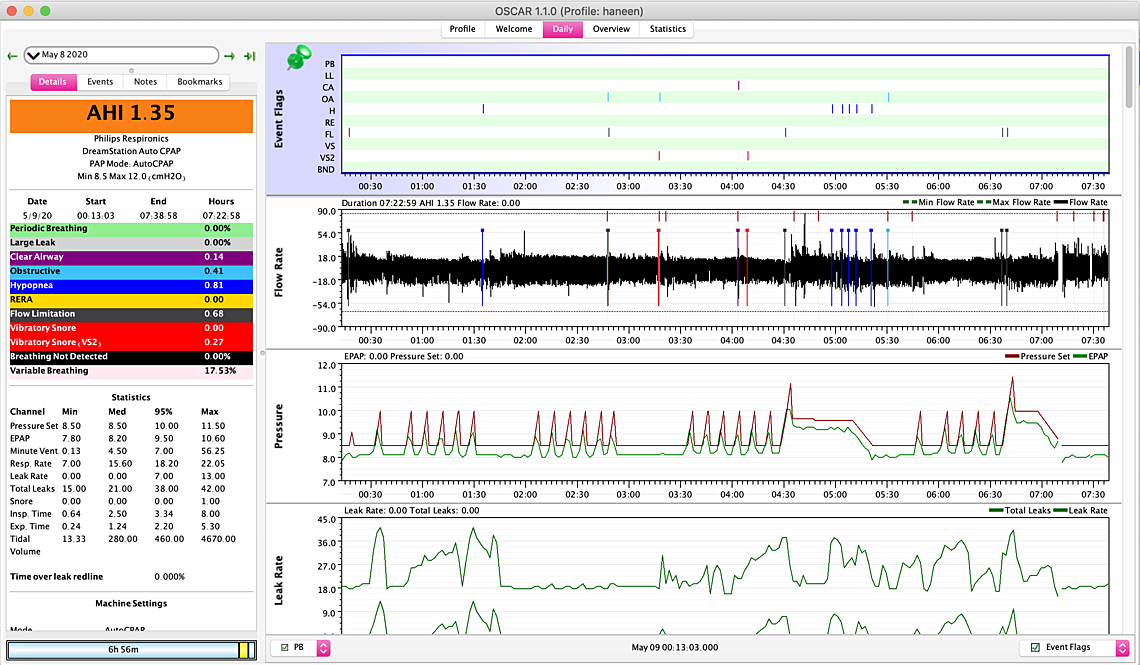
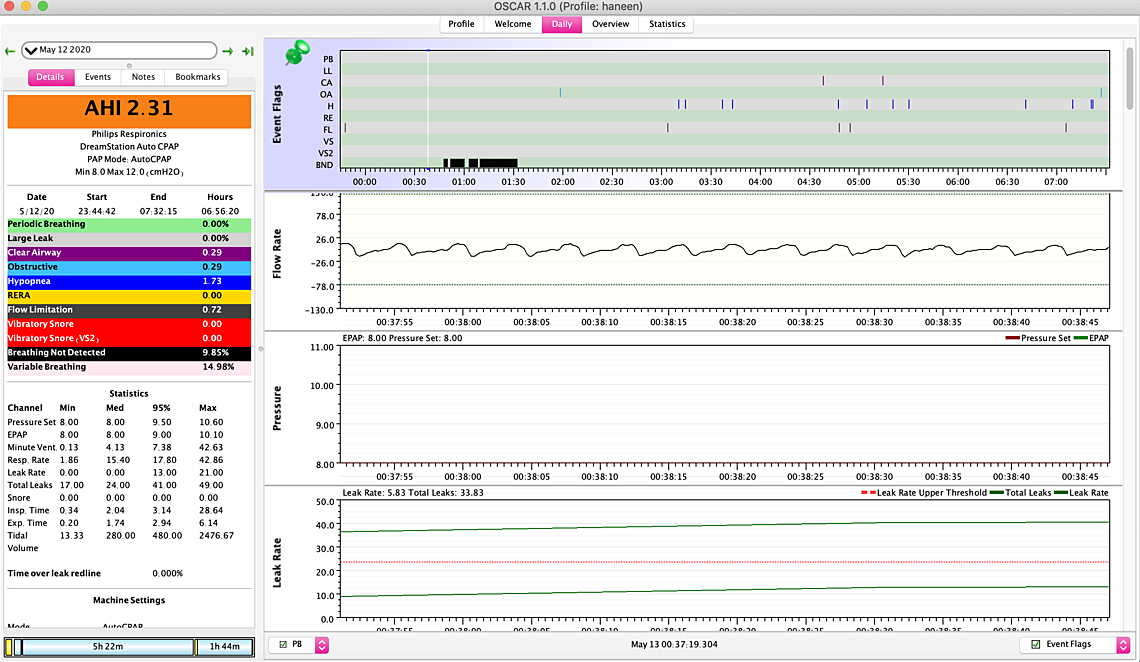
On May 8 I see the hypopneas and no real response in pressure. A hypopnea is a partial reduction in flow, and perhaps the DreamStation formula is to consider how my of a flow reduction there is and respond to more or less of a degree. It flagged it, so it must know it is there.
On the 12th there are some dark gray shaded areas that are flagged as BND or breathing not detected. That may be caused by your mouth open or your mask being displaced off causing a very large leak that the machine does not want to measure. You could try the mouth taping to see if it helps. Other than those areas I don't see any indication of high mask leakage. Make sure your machine is set with the mask type that matches the type of mask you are using. It uses that setting to compensate for the different purge leakage rates of each type of mask.
Based on your May 8 report, I would suggest increasing your minimum pressure up to 9.5 to see if that helps with the obstructive apnea and hypopnea. Don't see any excessive CA events, but you should watch that with the higher minimum pressure.
Oh ok I had no idea I could choose the mask type I'll figure that out tonight and slowly raise pressure ... thanks so much you have been a life saver...
It appears that Phillips uses a mask resistance setting from X1 to X5. If you are using a Phillips mask it should be stamped on the mask or in the user manual. If you are not using a Phillips mask you would have to figure out the probable X? setting for the best match of mask type. See this video for some help.
If you are still getting the migraines you might want to have your 02 levels checked while you sleep, your Dr should be able to provide a study order. I was told my headaches in the morning were because of my lack of oxygen at night. My sleep study showed me down to 63%. CPAP only raised it to 80%, and anything below 88 is a problem. They added supplemental oxygen to my CPAP and wow that made a world of difference for me. I now wear a Garmin Vivoactive 4 watch to sleep, it seems to be 1 to 3 points lower then a finger unit, but I now at least know when I go below 90% on my o2 levels. I turned my oxygen up to 2.5 and now my o2 rarely ever goes below 90 at night. The sleep information is interesting, the fitness stuff seems to be motivating me, but it will track my 02 levels the entire time I am sleeping and does not disturb me like the finger units do. Only 2 garmin watches will track all night. Beddrsleep has a device you tick you your forehead for $149 that tracks sleep data and O2 levels, only works with an iphone but is supposedly very accurate, and is trying to be approved for use in sleep studies since it tracks everything a home study tracks, but a lot less invasive. When they add android sometime this year I might get one. There are many good units you where on your fingers, but they prevented me from sleeping well which defeats the purpose and they lack the sleep data like movements, rem vs non rem sleep etc.. Good sleep data to match up to the CPAP data seems good to know.
hi Bigfootbitme thanks I will look into that.....
Sierra and (others) I have finally reached 9.5 but for some reason with the 9.5 last night I slept for ten hours and dreamt a lot which is weird because I never sleep that long but I woke up like at truck hit me (have been feeling horrible last few days even at the 9) - I thought I slept well but woke up feeling like a truck hit me... my throat is swollen from all the acid being sucked up even though I'm on Nexium... not sure where to go from here... I did switch from my nasal pillows to a cushion the pillows were bothering me... im wondering if that's the case even though I felt more comfortable with the cushions.. Also had two periodic breathings not sure if I should be worried I took a screenshot.. thank so much for your time!
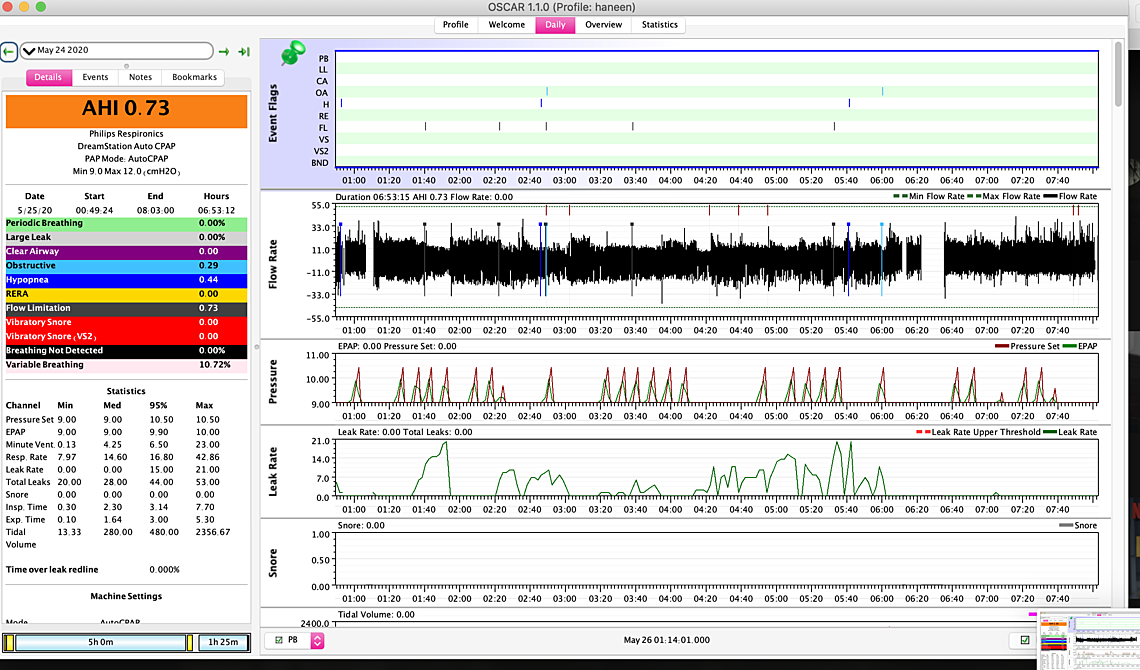
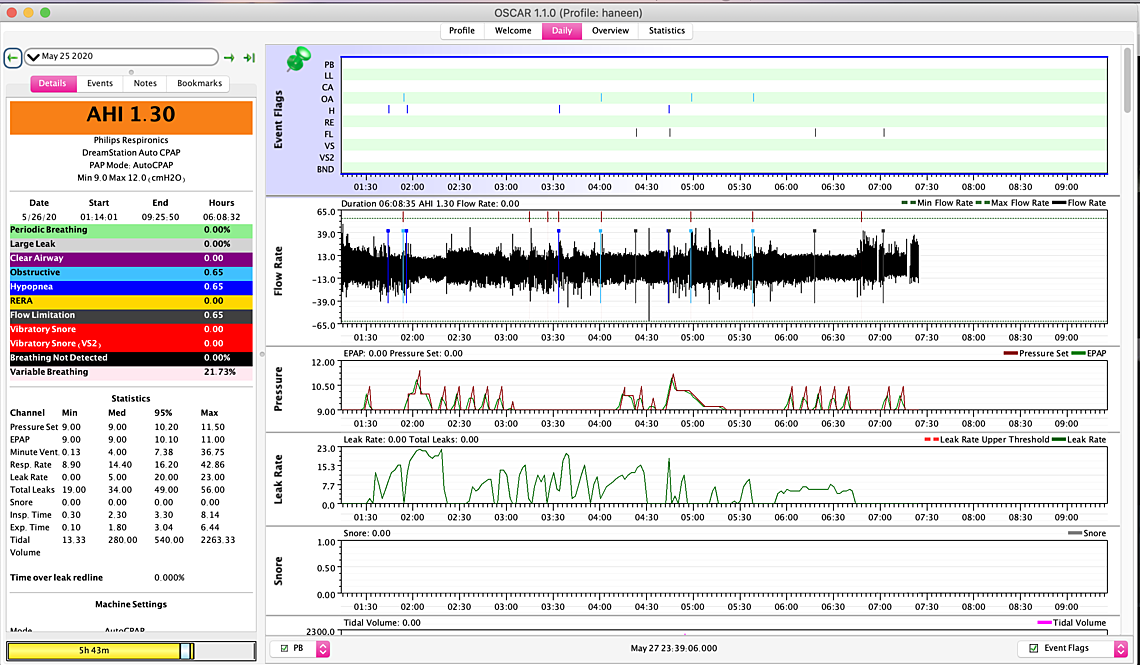
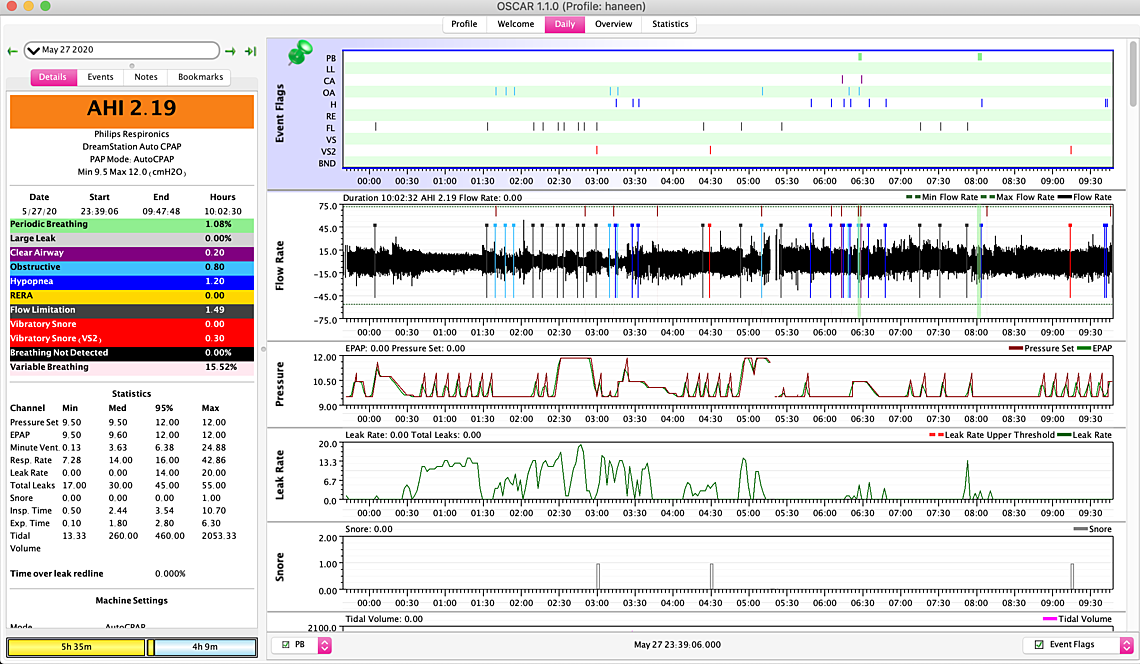
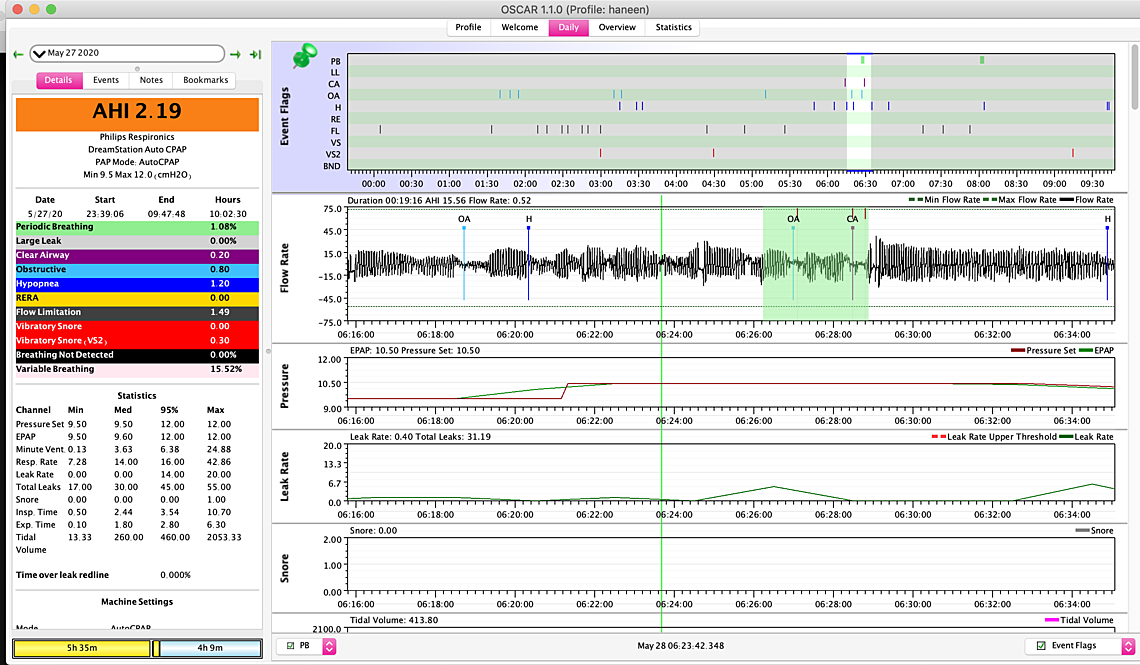
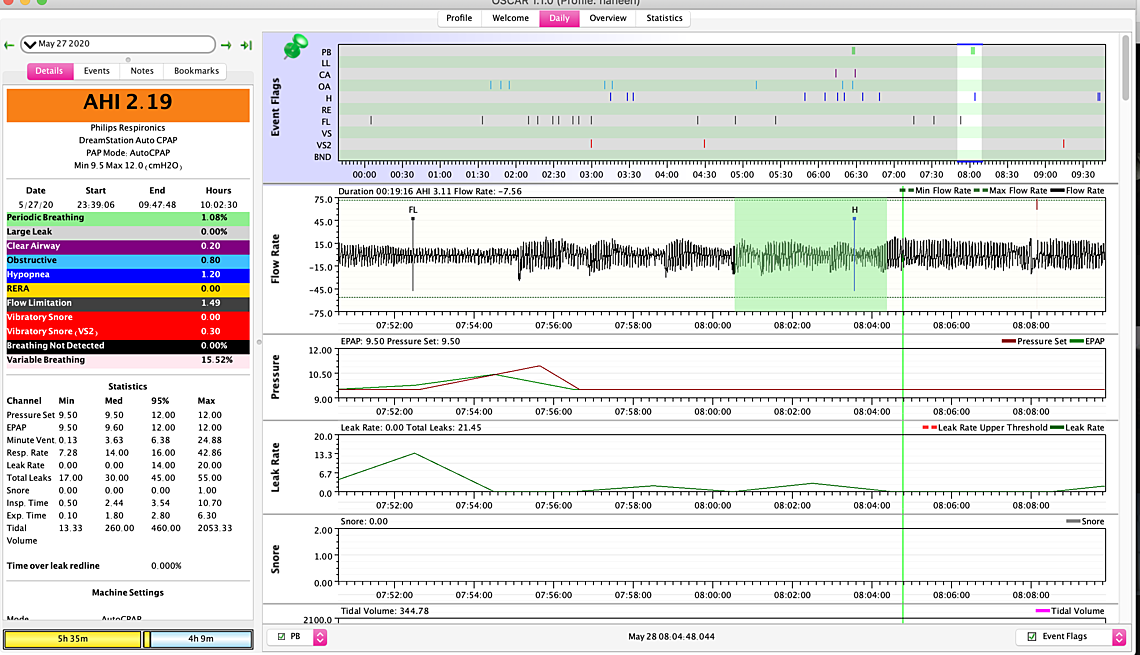
one more thing... I have turned my c flex off since last week.... I am wondering if turning it on would make me feel better? That's the only different thing that I have done besides increase the pressure... I am suspecting maybe the 8.5 or even the 8 (according to how I feel since its UARS) was better?
It is certainly not obvious that you are benefiting from the 9.5 cm minimum over the 9.0. I also see some CA events showing up. My thoughts would be to go back to the 9.0 minimum and perhaps a 10.5 maximum. I would try that for a week or so to establish an average which will be recorded in the Statistics tab. Then you may want to try try the Flex to see if it helps or hurts. I would go for the maximum Flex (3?) so the difference will be more obvious. When you set the 10.5 maximum you should check to see if there is any persistent pattern of events occurring when the pressure is limited to 10.5. If there are then it could be bumped back up a bit.
On the Periodic Breathing, that does not look like classic CSR. I would not worry about it unless it becomes persistent. CSR would have CA events between each breathing pulse, not OA.
The whole series of flow limitation events when at 12 cm pressure makes me wonder if you are having some head positional issues. Some claim significant benefits from using a soft cervical collar to keep the neck straighter during the night. You can get them at Walmart for $15 or so.
On switching mask types I have noticed some differences in that some masks seem to need more pressure to get the same results. I suspect that they really don't need more pressure, but the machine indicates that the pressure is higher. These machines do not measure pressure right at the mask, only in the machine. They only estimate mask pressure based on theoretical pressure drop calculation for the loss in pressure from the machine to the mask. So the bottom line is that in my experience anyway, a different mask design can change the required pressure that is indicated. It is a good idea to settle on a mask type and keep that part consistent during your testing for the optimum pressures.
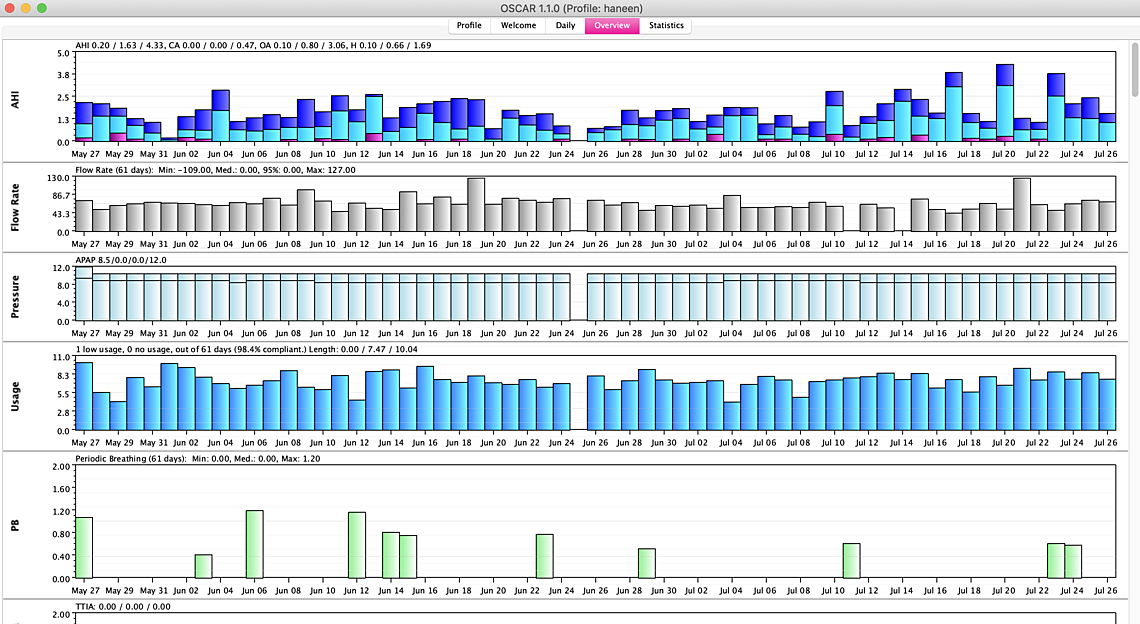
HI Sierra, thanks for your life saving advice! so its been a week I stuck to one mask and it seems that with this new pressure my numbers have reduced dramatically also have been sleeping longer- however I am still clenching away and waking up sometimes with burping and gas (only once in the middle of the night) I also still wake up with a headache and jaw clicking but do have more energy and feel better.... I am wondering though if I reduce it to 8.5 will it maybe solve the bloating/burping issue and maybe just to compare for a day or two if the 8.5 is better after reducing the maximum pressure... I am also getting at least one central showing up a day and I had another PB yesterday.... Do you think I should try it out for a few days.... I attached my weekly overview...... the numbers are better and I think I am sleeping more which is a good thing but was thinking for comparison and maybe to reduce the CA's maybe try it out for a few days? I still haven't played with epr at all .... let me know if you need to look at anything else.... Also my other suspect here in not feeling 100 percent (but thankfully feeling better) is maybe my LPR/GERD is playing a role (im on Nexium twice a day) I would be curious to know if it does affect apnea.... I have read that it has but no one knows which came first the chicken or the egg.... I also didn't know how to read what you said about if there is any persistent pattern of events occurring when the pressure is limited to 10.5-I wasn't sure how to read that... Thank you so so so much!
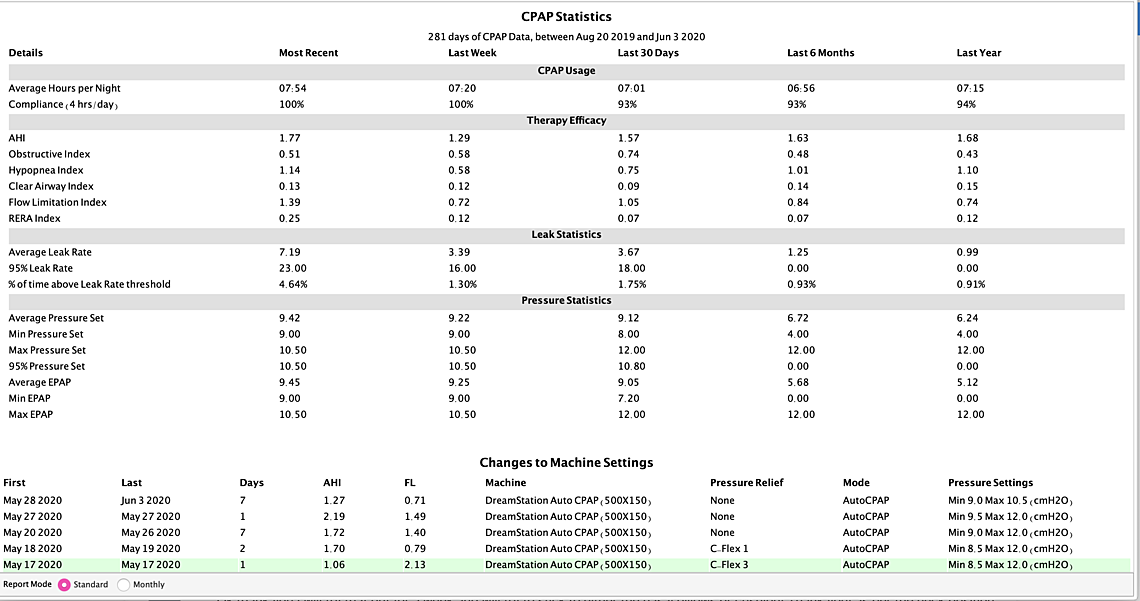
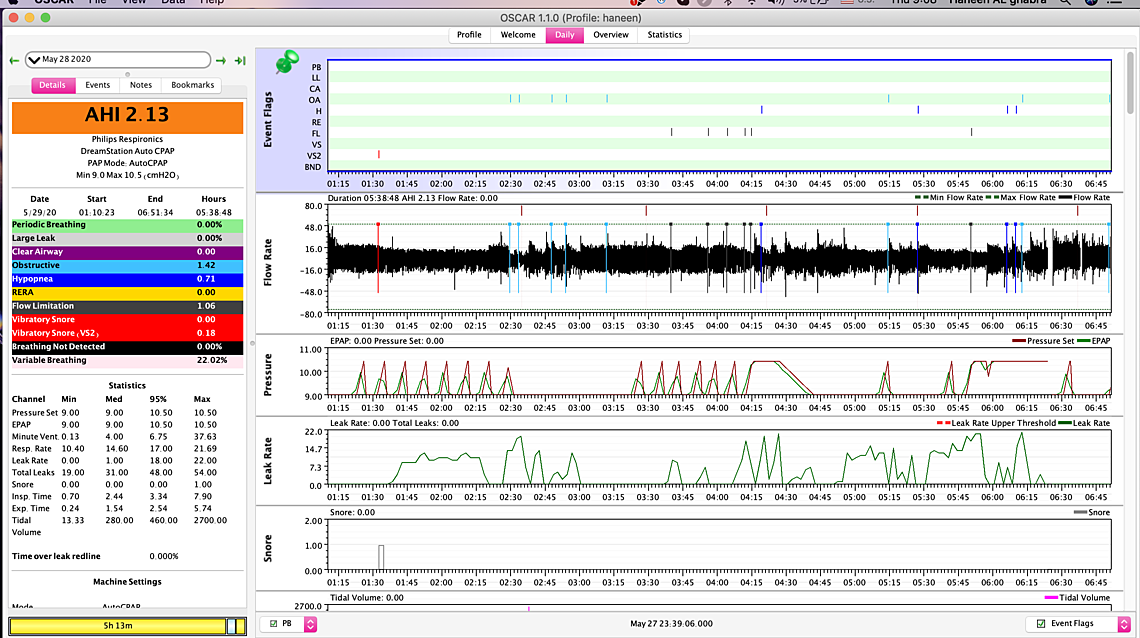
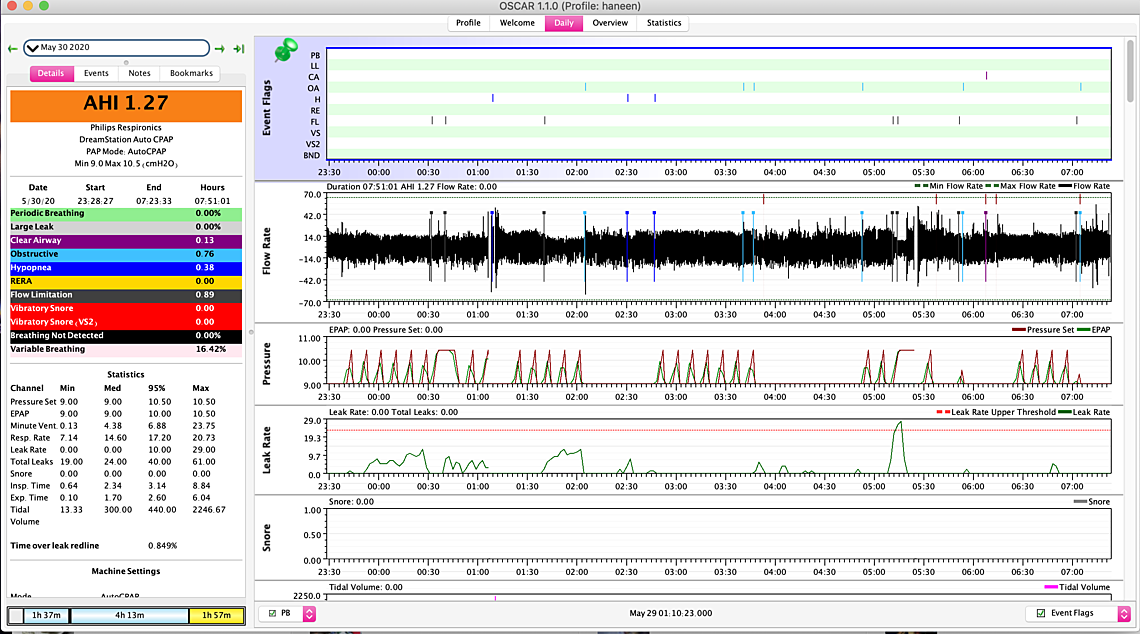
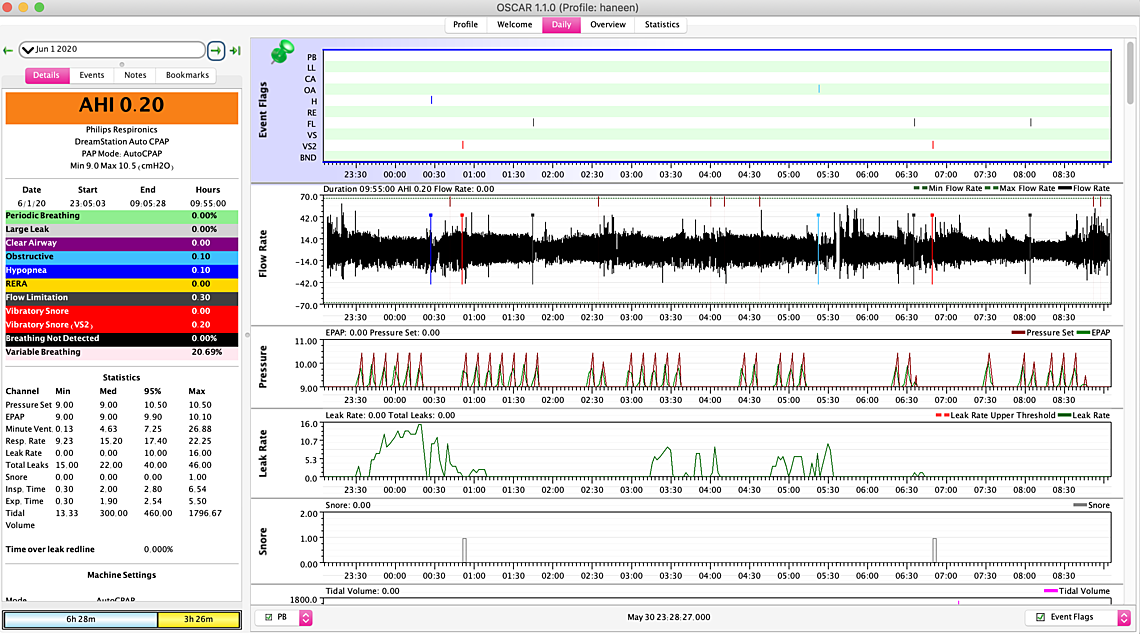
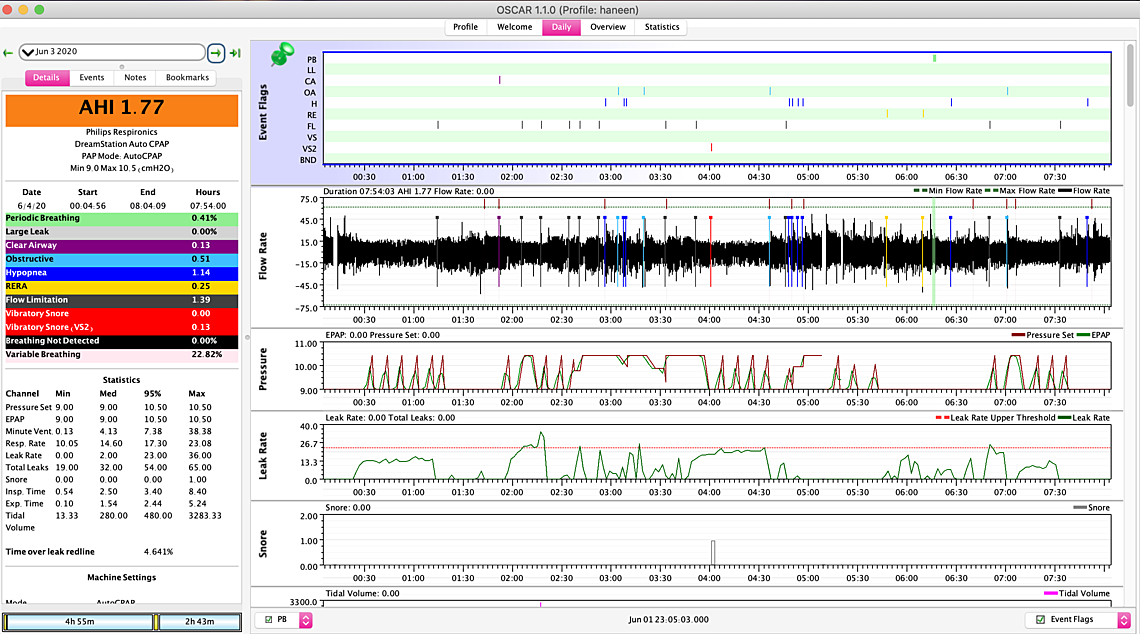
I think overall this is a pretty good setting. Not sure I would lower the minimum pressure unless you have to. There are a number of times when the pressure is at 9 cm and you are still getting some OA events. On limiting the maximum pressure to 10.5 there are some times when you are having events when the pressure is limited. They mainly seem to be flow limitations and hypopnea. I don't think limiting it is hurting you too much. Central events and PB do not seem to be a significant problem.
I think your options would be to try the Flex at maximum (3) without changing anything else. That should determine if it will help or hurt.
The other option to try would be to put the machine in straight CPAP mode and use a pressure of 9 cm. It is a bit time consuming to get the right pressure in CPAP mode, but with what you have done so far you are pretty close with 9 cm. After a week you could try 9.5 fixed or 8.5 fixed to see if they may be better. One upside of a fixed pressure is that the machine is not adjusting the pressure all the time. This may be more restful, if it achieves the same end result for AHI.
This all said, I would be pretty happy with what you have now. This is just a week of data, but your average is better than I can achieve.
Hi Sierra
I am starting to feel horrible again... I couldn't handle the bloating at 9 and my migraines and TMJ are back - I always wake up with a heart racing as well I am assuming from the obstructions for UARS .... the last two days I reduced the pressure from 9 to o8.5 due to all the bloating (all though it could really be my GERD and IBS flaring up and nothing to do with pressure I might try to goo back t that..... I felt good the first day after reducing to 8.5 and today feel bad again.... Iam keep thinking maybe I should try increasing the pressure to o12 again and see how that feels with the 8.5? I am not sure - also the heart racing is scary but in the past I have done tests and there was really nothing wrong with my heart....
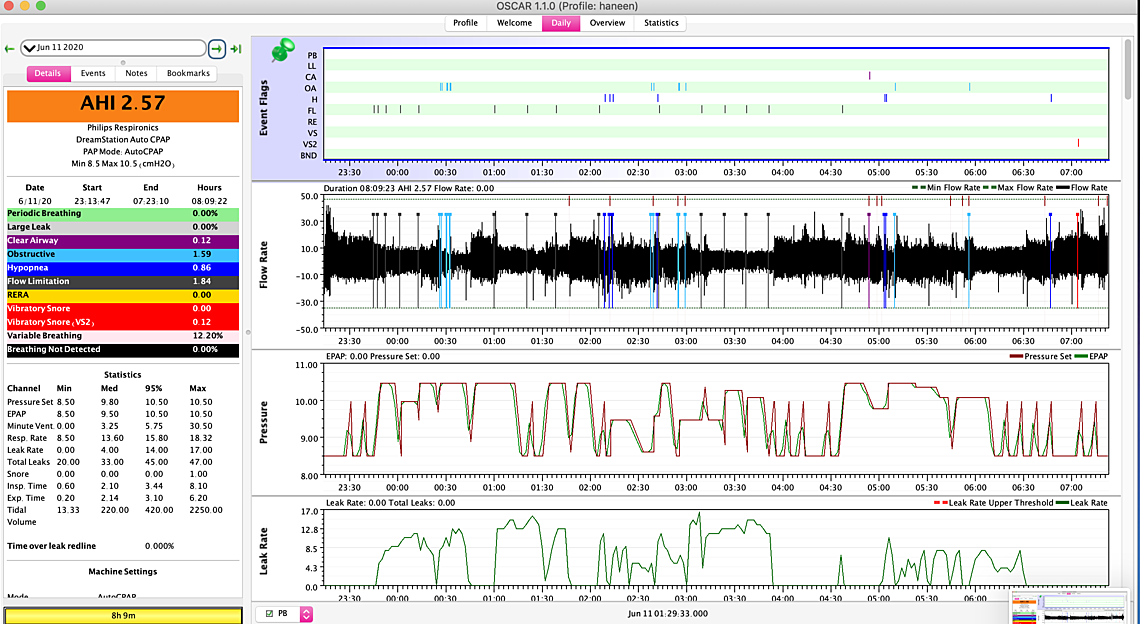
There should not be much difference between 9 cm and 8.5 for a minimum pressure. Going up in pressure usually makes the air swallowing issue worse, not better. Have you tried the Flex back on again at 3? I am not sure how it would help, but since it is there, it is worth a try to see what it does.
The other option is to switch the machine into basic CPAP mode and pick a pressure to try. I would suggest 9 cm to see what you get. From there you could try lower or higher. The one advantage of CPAP mode is that you will not have the pressure cycling up and down all night long. Flex should also work in CPAP mode if you want to try that as well.
HI Sierra
So I was fine for a while especially that my doctor increased my Nexium dosage (it helped a lot) more good days then bad so I am still at a loss at what came first the egg (the apnea) or the chicken (then acid reflux). nonetheless the last four or five days have been horrible again. I don't get why its getting worse again but I attached some of my charts. Thanks so much for your help
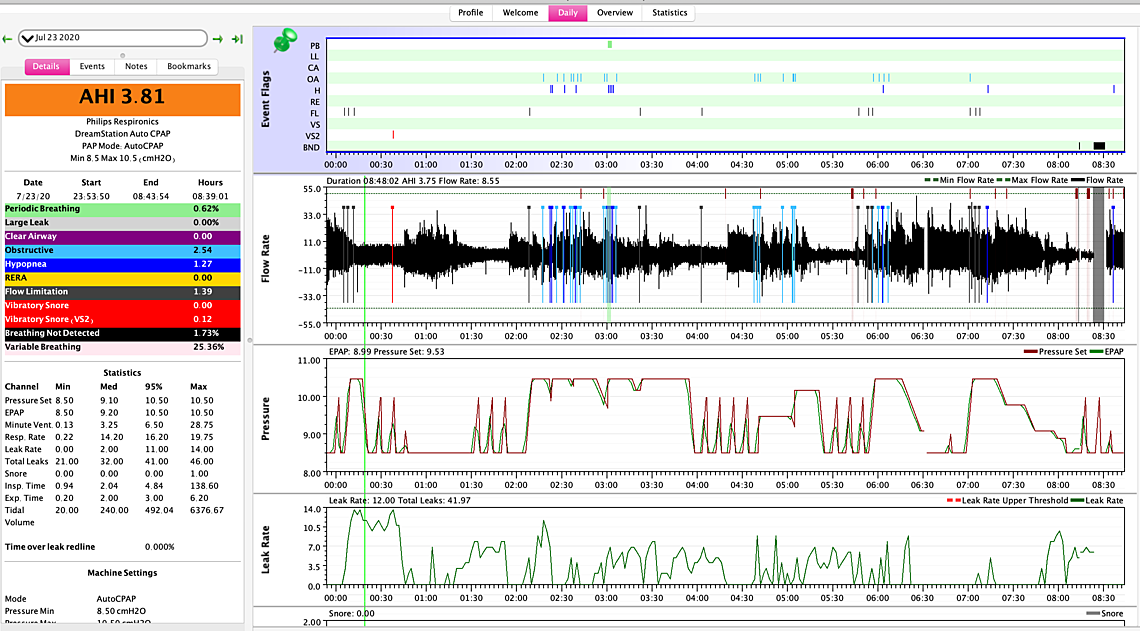
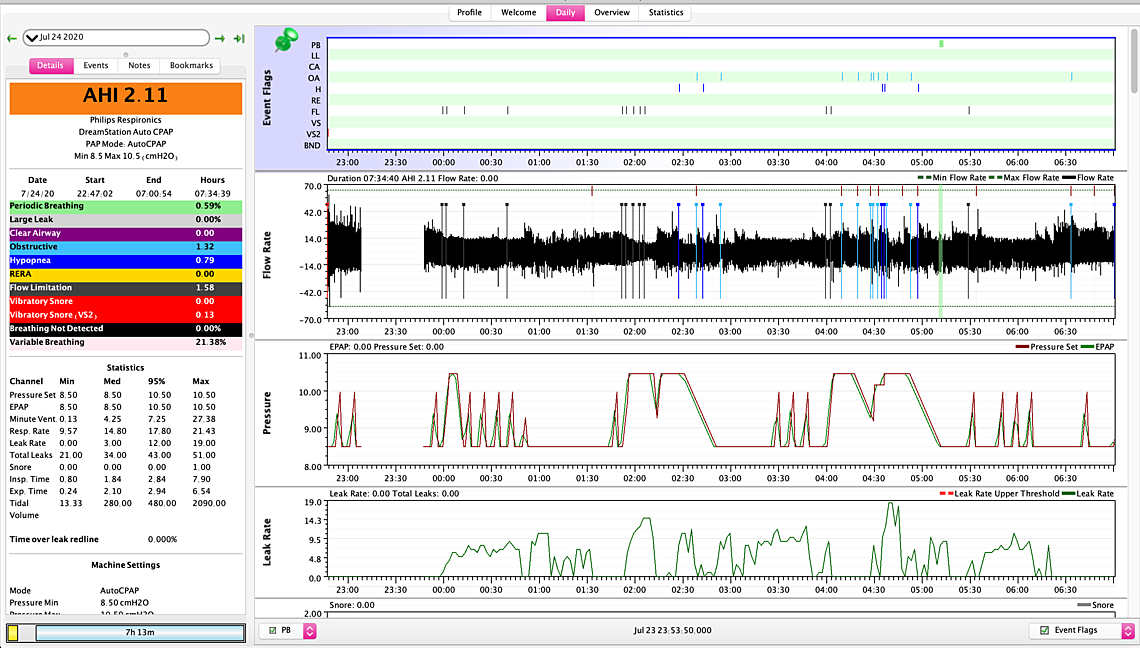
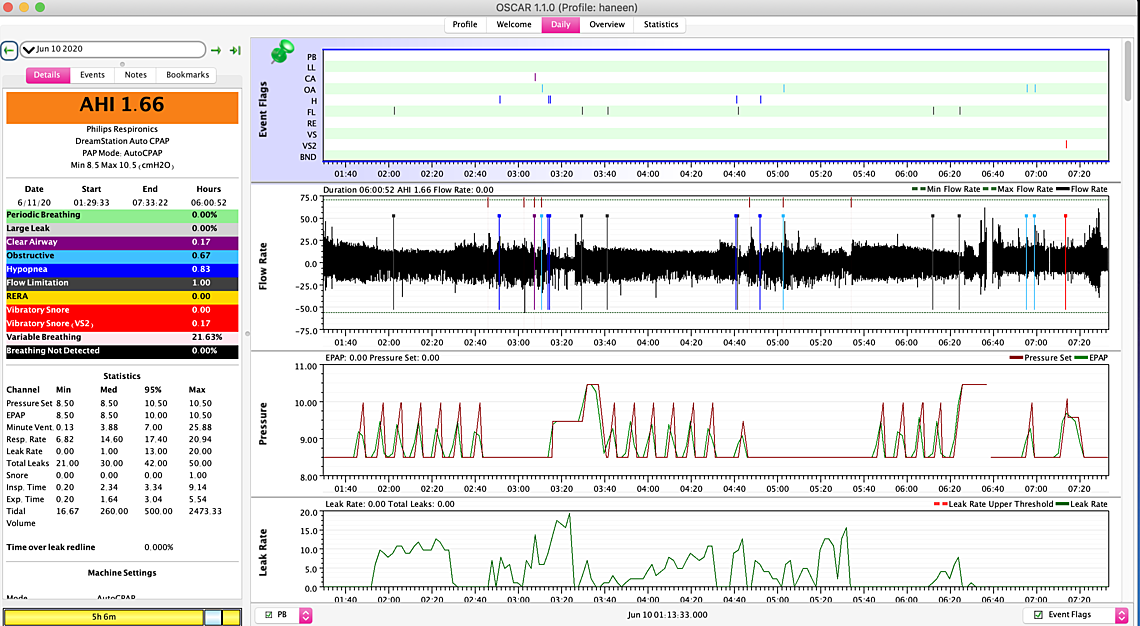
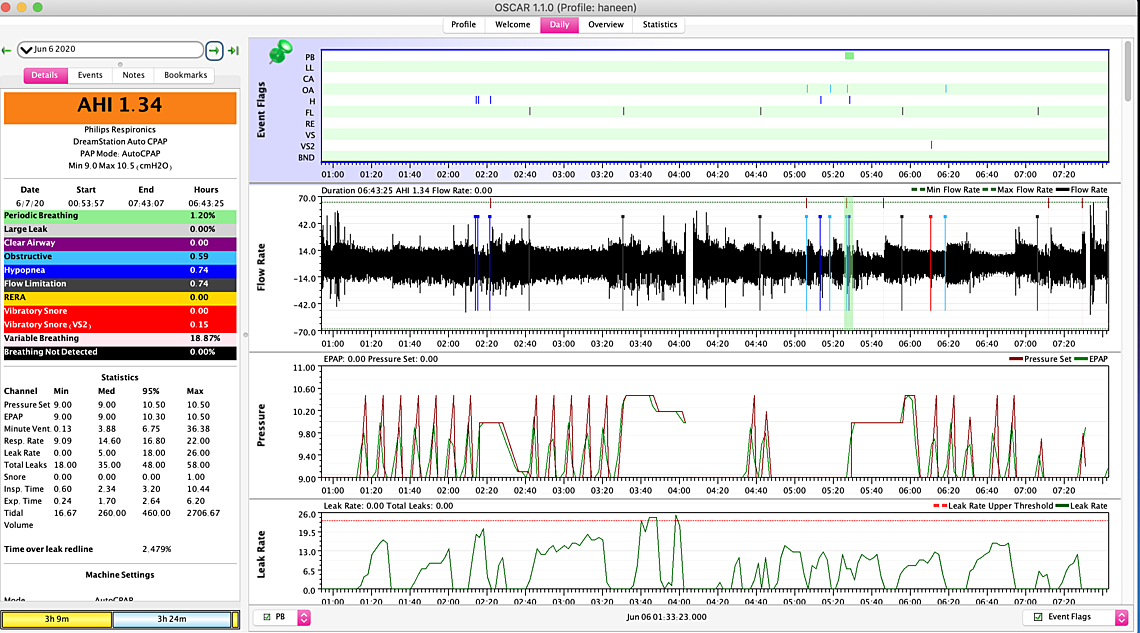
The first one with the AHI of 3.81 appears to have most of the obstructive events at the higher 10.5 pressure. One would have to expand out the time scale to see what pressure each one was at when it happened. But if they are all at the higher pressure that suggests the maximum could be increased to help avoid as many of them.
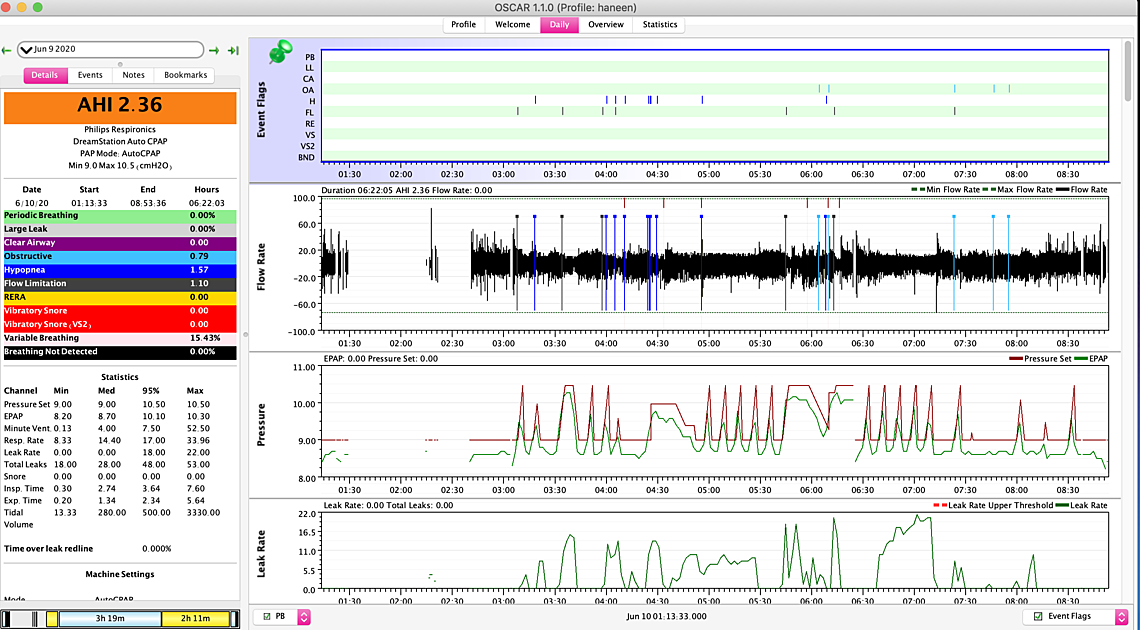
The second graph with AHI of 2.11 seems to have some events happening at the lower 8.5 pressure. That would suggest the minimum may need to be increased.
In both nights there does not seem to be much central apnea, so these pressures don't seem to be a problem where they are now with respect to clear airway events.
Hi does this help? what do you suggest I change the pressure to? perhaps 9 to 12? or to 11? 
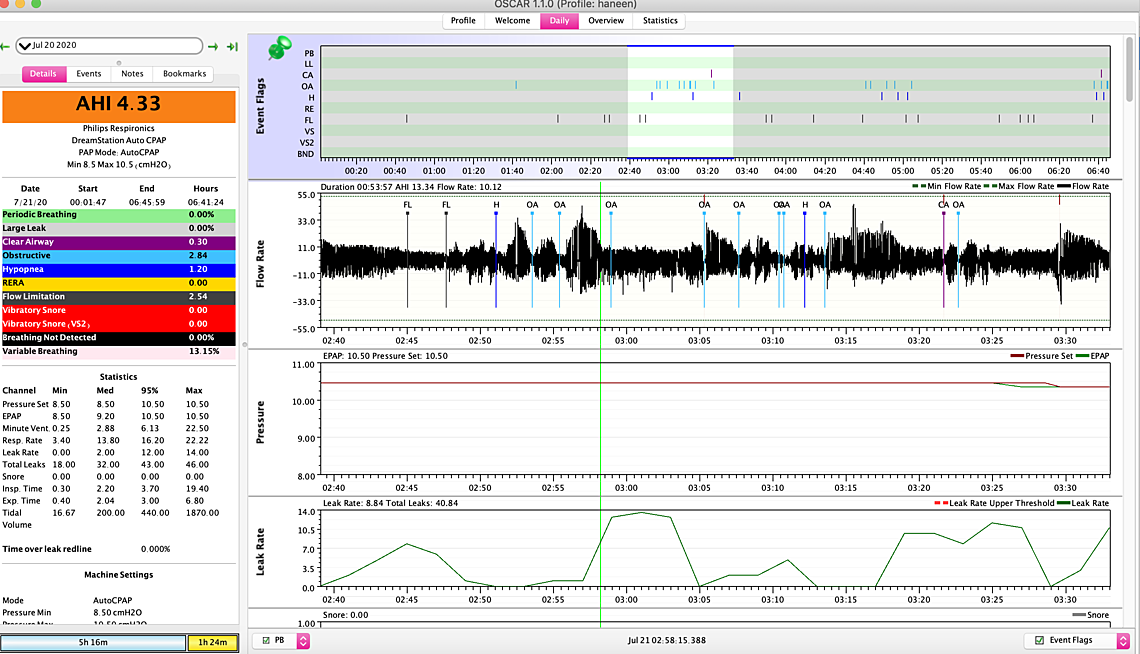
Yes, both of those screen shots suggest you could benefit from a higher maximum The only down side of more pressure in this range is the risk of initiating CA events. This does not appear to be the case, from these charts, but it is something to watch. I would try 11 or 11.5 to see if that helps.
There is also the possibility that I think we discussed before that it is a positional issue which might be helped with a soft cervical collar. I say that because the events are clumped together.